INTRODUCTION
Spontaneous subdural empyema is a rare disease in developed societies and is even rarer in adults than in children. The most common cause of spontaneous subdural empyema in adults is paranasal sinusitis caused by Streptococcus pneumoniae10). The treatment for subdural empyema is not yet established, although surgical treatment and antibiotic treatment are common.
We examined the efficacy of continuous irrigation and drainage catheter insertion through the following case.
CASE REPORT
A 30-year-old male was brought to our hospital by ambulance in stupor. He had experienced fatigue and paralysis of his right side for a couple of days. A day prior to visiting our hospital, the patient’s consciousness had then deteriorated into stupor and was unable to communicate. However, the patient’s parents delayed their visit to the hospital for more than 24 hr because they thought the patient would recover. The patient had a history of schizophrenia and had undergone several surgeries for sinusitis. When the patient arrived at the emergency room, his consciousness was in a state of stupor, both pupil reflexes were sluggish with 3mm diameters, and right side paralysis was Grade I. Body temperature was 39.4°C and blood pressure was 120/80mmHg, Heart rate was 110 beats/min and respiration rate was 12 breaths/min. Laboratory findings showed C-reactive protein (CRP) 23.33mg/dL, white blood cell 15,440/μL (Segment neutrophil 85.7%), erythrocyte sedimentation rate (ESR) 95mm/hr, activated partial thromboplastin time 37.8 sec, prothrombin time (PT) 15.3 sec, and international normalized ratio 1.21.
In computed tomography (CT) scans (Fig. 1), a fluid-fluid layer with heterogeneous density was seen in the subdural space of left cerebral convexity and pneumocephalus around the falx. However, we have only diagnosed the chronic subdural hematoma and subacute subdural hematoma with neglect of this pneumocephalus.
We concluded that it would be difficult to treat this patient with burr hole (BH) trephination because of his diagnosis of chronic subdural hematoma and subacute subdural hematoma, therefore a craniectomy was planned and performed immediately.
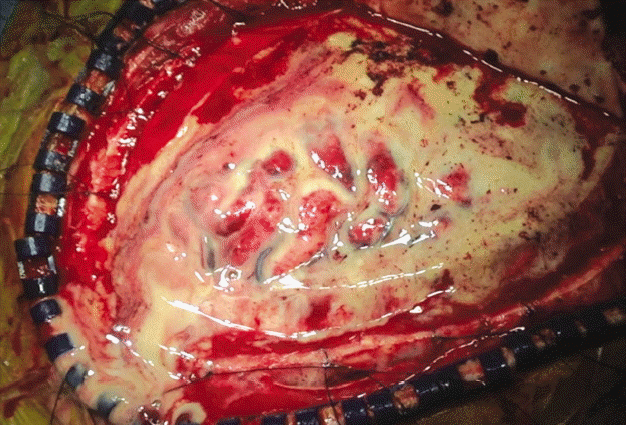
However, when we examined the subdural space during the operation, it showed yellowish pus instead of hematoma (Fig. 2). Therefore, we cultured the pus, performed massive irrigation through normal saline, removed the pus, and finished surgery using a continuous irrigation and drainage catheter instead of a Hemovac.
After the operation, the patient was transferred to the intensive care unit (ICU) and the continuous irrigation and drainage catheter maintained for 8 days with midazolam for catheter maintenance.
The infusion rate of continuous irrigation and drainage was maintained at 20cc/hr on the first day and 10cc/hr on the second day. We were planning to wean the irrigation by gradually reducing the rate, but the patient began to have seizures as the infusion rate was reduced. We determined that the pus was not cleared well, which caused stimulation of the brain cortex, resulting in seizures, which consequently led us to increase the infusion rate to 30cc/hr. Until the culture results from the operation were confirmed, we used third-generation cephalosporin and metronidazole as empirical antibiotics. Five days after the culture, Streptococcus anginosus was identified and metronidazole was replaced with vancomycin after confirming susceptibility test results.
On post-operative day (POD) 10, endoscopic sinus surgery was performed to treat chronic sinusitis, which was considered the likely cause of the subdural empyema. A culture test was also performed during this surgery and Streptococcus angionosus was identified.
On POD 14, a follow-up CT confirmed that the pus around the falx had reappeared, and a second operation was performed. A BH was drilled in the frontal area, and an additional craniotomy was performed in the occipital area for irrigation and removal of pus. A continuous irrigation and drainage catheter was attempted once again, but the space was very narrow and adhesion was severe, thus, only simple irrigation was performed and the operation completed.
The patient’s consciousness and paralysis slowly recovered the day after the second operation. His right side paralysis had improved from Grade I to III on POD 7.
The pus was mostly absent from the follow-up CT obtained on POD 14 of the second operation. The patient continued to receive rehabilitation treatment and was re-admitted for cranioplasty two months later. The patient’s consciousness was restored to an alert state and the right side paralysis also recovered.
Cranioplasty was performed using a titanium mesh as autologous bones could not be used due to infection. About three months later, his consciousness and paralysis had been fully recovered.
DISCUSSION
Subdural empyema is a rare disease6). Subdural empyema can be found in all ages, but it is found more commonly in men, and the causes are different in each age group. Subdural empyema occurs in infants and children as a complication of bacterial meningitis. Paranasal sinus disease and otitis media are common causes in adolescents and adults1,7,10).
Iatrogenic procedures (craniotomy, subdural hematoma drainage), penetrating head trauma, and seeding from distant infection sites (endocarditis, sinusitis) can also cause subdural empyema6,7,10). Streptococcus anginosus is found in many parts of the human body and can cause chronic pansinusitis. In our case, Streptococcus anginosus was identified in the first bacterial culture test for the first operation, and then both Streptococcus anginosus and Staphylococcus haemolyticus were identified in the bacterial cultures performed during otopharyngeal surgery. In general, aerobic and anaerobic Streptococci are the most common organisms causing subdural empyema2,4,7,10) as in our case in which Streptococcus angionosus was cultured. Streptococci often cause sinusitis. The patients had undergone several sinusitis surgeries. We concluded that pansinusitis was the cause of subdural empyema in our patient, because the same bacteria were identified in culture results of neurosurgery and otolaryngology surgery (Fig. 3).
Subdural empyema is very dangerous because neurological symptoms can progress rapidly with a mortality rate of 2% to 12%5,7,9). However, treatment of subdural empyema remains controversial6,10). It is common to combine antibiotic therapy with surgical treatment. For antibiotic treatment, broad-spectrum antibiotics (third-generation cephalosporin, vancomycin, and metronidazole) are used1,10) and the general duration of treatment is 3 to 4 weeks2). However, subdural empyema is difficult to treat with antibiotic treatment alone because it is difficult for antibiotics to enter the subdural space. In most cases, surgical treatment is necessary. There is no established treatment when it comes to surgical treatment, but simple drainage of pus through a craniotomy or craniectomy is commonly used8). The continuous irrigation and drainage that we performed is helpful for the rapid and continuous removal of pus, especially when the pus is adhesive3). Continuous irrigation and drainage has the advantage that it can clean the areas that simple irrigation is unable to reach. In our case, the pus was well controlled while maintaining the continuous irrigation and drainage catheter. Although a second operation was performed due to a focal recurrence of pus, there wasn’t further recurrence afterwards. The results of our patient treated with this method were very satisfactory with good recovery.
Because subdural empyema is very rare, it is important to suspect and differentiate it from subdural hematoma. We initially diagnosed the lesion as a subdural hematoma because thorough patient evaluation was difficult at the time of the initial diagnosis as the patient was in an emergency situation, and we believe that neglecting the pneumocephalus that was found in the first CT is the cause of misdiagnosis (Fig. 4). Magnetic resonance imaging (MRI) would have been helpful if we had had suspicions of subdural empyema and had planned to perform additional tests.
CONCLUSION
As the incidence of subdural empyema is very low, it is important to suspect subdural empyema to avoid a misdiagnosis. If subdural empyema is suspected, MRI and laboratory findings (CRP, ESR, etc.) would be helpful. After diagnosis, antibiotic treatment and surgical treatment should be combined for effective treatment. We performed short-term continuous irrigation and drainage catheter insertion and systemic antibiotic treatment satisfactory results. If a patient is confirmed to have sub-dural empyema, we believe short-term continuous irrigation and drainage catheter insertion and systemic antibiotic treatment may be helpful.