INTRODUCTION
Since the initial description of lumbar disc herniation by Mixter and Barr, lumbar discectomy has become the gold standard of microsurgical treatment for lumbar disc herniation. But, large central extruded disc herniation is difficult to treat successfully.
In cases with a mild symptom such as only tolerable low back pain, conservative treatment is usually recommended. But surgical intervention is required in cases of severe low back pain with or without lower extremity radiculopathy in spite of consistent conservative treatment. Several techniques have been reported for large central extruded disc herniation. Wide laminectomy or bilateral partial hemi-laminectomy is required for adequate decompression, but it entails the risk of spinal instability. To deal with instability, most of the authors have recommended lumbar fusion2,8,10). But there are inherent fusion-related problems, such as adjacent segment degeneration, back muscle atrophy, failed back syndrome, and decreased range of motion3,7,9).
Hence, we adopted the bilateral decompression with unilateral laminotomy technique that is mainly used for degenerative lumbar stenosis. Through this method, a large central disc can be removed totally by bilateral discectomy with the CO2 laser. To illustrate this minimally invasive technique, we describe two cases that underwent this procedure and its pros and cons with review of the literature.
MATERIALS AND METHODS
Among the patients with herniated nucleus pulposus in the lumbar spine, selected cases fulfilled the following inclusion criteria: (1) a large central disc that compresses the spinal canal; (2) refractory to consistent conservative treatment for more than 3 months; (3) no instability on the preoperative dynamic flexion-extension radiography; (4) no severe arthropathy; (5) a relatively young and middle-aged patient.
A large central disc was removed via BDUA with the CO2 laser and magnetic resonance (MR) images was taken to confirm adequate decompression on the first postoperative day. Serial X-rays were taken to identify possible instability and the clinical outcome was measured using the visual analog scale (VAS).
1. Operative Technique
We used the modified minimally invasive technique, unilateral laminotomy with contralateral decompression. The patient was placed prone with marked flexion (the knee-chest position that is the standard for microdiscectomy) in a Wilson frame under spinal anesthesia. The paraspinal muscles were detached from their bony attachments on the spinous process and lamina to expose the bony structure. After positioning the standard Caspar retractor, the microscope was brought into the operative field. Then, the operating table was elevated, tilted to the opposite side of the operator by about 30-40 degrees. Microscope was also tilted towards the opposite site at a proper angle. This maneuver is a key factor for adequate visualization of the ipsilateral and contralateral side at the same time across the midline beneath the deepest portion of the interspinous ligament.
Using a high speed drill (HiLAN®, Germany), the operator created a thin bony structure on one side of the cranial lamina. Then, the thinned out lamina was removed with 2 or 3 mm Kerrison punch until the ligamentum flavum(LF) was exposed. The thinning and removal of lamina was performed up to the upper border of the LF. Contralateral partial hemi-laminotomy with a high speed drill on the inner side of laminae was performed at the same time using the midline cleavage between the LFs as a landmark. With tilting of the operating table and microscope as described in the previous paragraph, this was performed easily by preoperative measurement of the drilling distance. Drilling on the contralateral side was performed above the LF to protect the thecal sac. Additionally, great care was taken not to detach the spinous process completely. Drilling was performed until the contralateral superior and inferior articular processes were visualized. This made it easier to perform foraminotomy. Caudal laminae were also drilled out in a similar fashion. After bilateral laminotomy, the LF was removed with Kerrison punch. Especially, a small sized (ex. 2 mm sized) Kerrison punch is recommended for removal on the contralateral side. For removal of a large central extruded lumbar disc, we used the CO2 Laser (UltraPulse®, Lumenis Co, Israel) connected to the operative microscope. When using the CO2 laser, about 300 joules of laser energy was used. With the CO2 laser, annulotomy was performed easily despite the relatively small space. After ipsilateral discectomy, gentle retraction of the dura by a root retractor with a cottonoid was performed, and the contralateral side disc was easily visualized. During CO2 laser treatment, heat injury was prevented by frequent cooling with saline irrigation and/or protection with barriers such as cottonoids. After bilateral microdiscectomy was performed, the wound was irrigated, bleeding points were coagulated, and the wound was closed in layers with sutures.
RESULTS
We performed minimally invasive surgery for a large lumbar central extruded disc. All patients had no intraoperative complications such as dura mater injury, root injury etc. and they showed improvement in the clinical outcome and total removal was confirmed on the first postoperative day MR images. Follow-up X-ray showed no aggravation of spinal instability. Among the cases, we present 2 cases with radiological and operative findings.
1. Case I
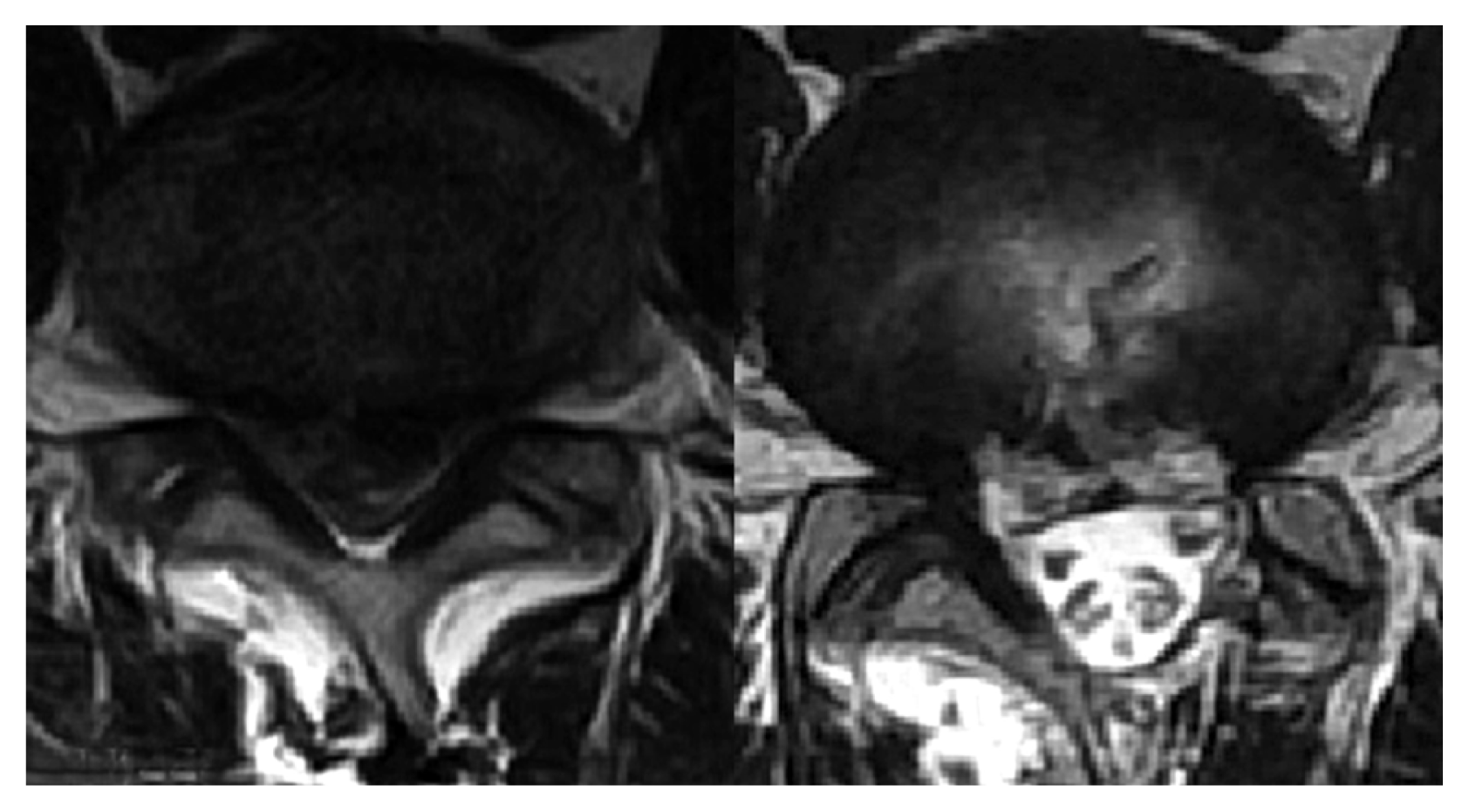
A 42-year-old man presented with low back pain and pain in both legs. The VAS score was 8 out of 10. On neurological examination, the patient showed decreased ankle dorsiflexion power (Rt. Gr II/ Lt. Gr I) and hypesthesia in both L4, 5 sensory dermatome areas. He also complained of difficulty in urination. Magnetic resonance images revealed a large lumbar extruded disc at L4-5 (Fig. 1). He underwent operation with the BDUA technique. Completed discectomy and neural decompression was confirmed on the first postoperative day MR images (Fig. 3) and VAS score decreased to 3 out of 10. But, the motor and sensory deficit was slightly improved. The patient is currently undergoing a rehabilitation program.
2. Case II
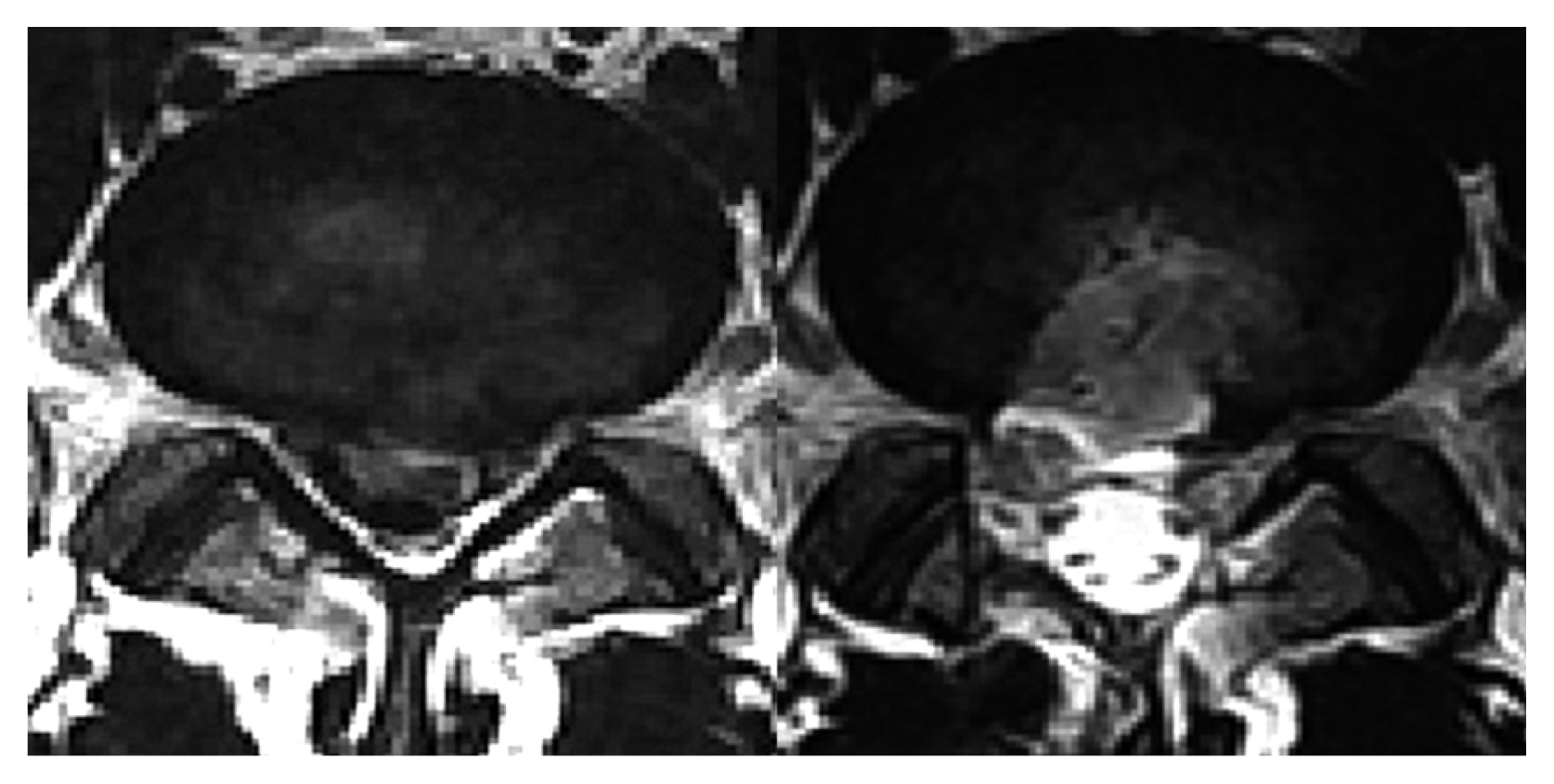
A 23-year-old man presented with a 4-year history of low back pain and radiating leg pain. The VAS score was 6 out of 10. He had undergone MR images 4 years ago. MR images revealed a moderate central extruded disc at L4-5 and L5-S1. Despite consistent conservative treatment, his symptoms did not improve and we reassessed MR images. MR images revealed a diminished extruded disc at L4-5, but a more aggravated disc at the L5-S1 level (Fig. 2). We performed operation via BDUA at the L5-S1 level. Complete disc removal and neural decompression were confirmed on the first operative day MR images (Fig. 2). VAS score decreased to 2 out of 10. At the last follow-up 3 months after surgery, his low back pain and radiating pain had resolved and no instability was seen on dynamic radiography.
DISCUSSION
Lumbar discectomy as the surgical treatment of disc herniation has certainly evolved since the initial reports of this disease entity more than 70 years ago. But in the Medline database, there are only some reports of a large central disc. There are possible concerns regarding the treatment of a large central lumbar disc; nerve root injury due to severe root distraction, inadequate disc removal, and possible spinal instability.
Conventional unilateral laminotomy with discectomy alone is inadequate to treat a large disc. There is much more tension on the root and dural retraction to remove the disc completely.
Total discectomy via total laminectomy or bilateral laminotomy can remove the disc totally without nerve root retraction injury but possible instability ensues. Most of the authors have recommended fusion to deal with this problem. But there are inherent fusion related problems; paraspinal muscle atrophy, adjacent segment disease, decreased range of motion1-4,6,7).
We adopted the unilateral laminotomy with bilateral decompression technique for creating adequate space for total removal of a large disc. Unilateral approach that preserves the facet joints, neural arch of the contralateral side and contralateral paraspinal musculature decreases the risk of postoperative destabilization and protects the nervous structure against posterior scarring5).
Another main concern for spine surgeons with respect to less invasive techniques for a large disc is nerve root injury during nerve retraction and decompression. As in spinal stenosis, careful drilling of the cranial and caudal laminae to keep the LF intact is a key factor. The LF protects against neural injury during decompression.
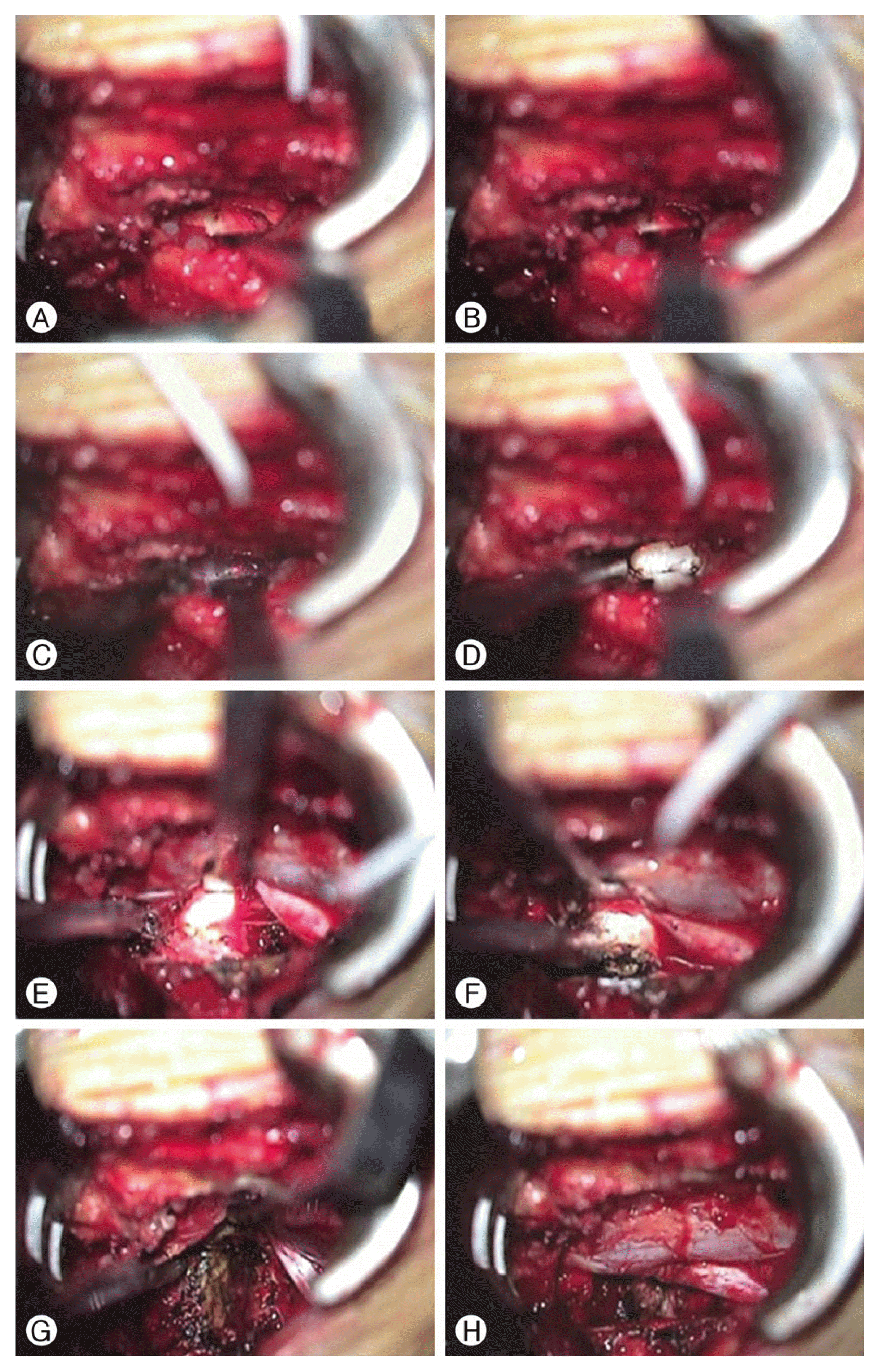
After the removal of the LF, the contralateral traversing root and dura were observed within the microscope field of view. Although adequate room was created by contralateral drilling, there was a relatively small working space because the large disc compressed the dura and root. We used the CO2 Laser (UltraPulse®, Lumenis Co, Israel) to deal with this problem. After ipsilateral discectomy, gentle retraction of the dura by a root retractor with a cottonoid was performed, and the contralateral side disc was easily visualized. Contralateral annulotomy can be easily performed with the CO2 laser. The CO2 laser seems to be of great benefit in discectomy especially in foraminal disc or contralateral discectomy. As shown in Fig. 3, it does not obscure the surgical microscopic view, and surgeons can easily perform discectomy without significant root retraction.
Based on our experience in the above 2 cases, in which BDUA was performed, the results were quite promising. We agree that a large central disc with segmental instability can be an indication for fusion9). Although this technique needs further validation by including more cases and long-term follow-up, the preliminary results indicate that this technique can be an effective alternative option for a large central disc, especially in the young and middle-aged patients without inherent fusion-related problems.
CONCLUSION
In this report, we describe a new technique for a large central lumbar disc. Although a large number of cases are needed, this technique may be relatively easy and have a short learning curve. This technique can be an effective alternative option for a large central disc, especially in the young and middle-aged patients without inherent fusion-related problems.