Cerebral Myxomatous Aneurysm Treated by M2-M2 Bypass: A Case Report
Article information
Abstract
Intracranial aneurysms associated with atrial myxoma have been reported and termed “myxomatous aneurysms.” We present a case of cerebral myxomatous aneurysms treated by M2-M2 bypass surgery. A 20-year-old woman was admitted for evaluation and management of multiple cerebral aneurysms found incidentally. She had a history of right middle cerebral artery (MCA) territory infarction with MCA total occlusion. At that time, cardiac myxoma was incidentally found and surgically removed. In cerebral angiography, multiple cerebral aneurysms were identified. Among them, a right MCA fusiform aneurysm was the largest, with a diameter of 19.5 mm; notably, this developed at the site of previous MCA occlusion. Through surgical exploration, an MCA bifurcation aneurysm was observed, with a permanently occluded inferior trunk toward the temporal lobe. M2-M2 end-to-end anastomosis with resection of aneurysm was successfully performed, and biopsy showed dilation and thickening of the aneurysmal wall without any evidence of tumor invasion. The outcome of this case shows that surgical resection with bypass surgery is a useful option for the treatment of cerebral myxomatous aneurysms.
INTRODUCTION
Intracranial aneurysms associated with atrial myxoma have been reported and termed “myxomatous aneurysms”. Because of their infrequent incidence, treatment strategy for multiple myxomatous aneurysms is not well-established. Here, we present a case of cerebral myxomatous aneurysms in our hospital treated by M2-M2 bypass surgery.
CASE REPORT
A 20-year-old woman was admitted to our institute for evaluation and management of multiple cerebral aneurysms that were found incidentally. She had a history of sudden onset of left side motor weakness 4 years prior; magnetic resonance (MR) angiogram had confirmed right middle cerebral artery (MCA) total occlusion, with MCA territory infarction. Intravenous tissue-type plasminogen activator and thrombolysis was administered, and the MCA was recanalized. Echocardiography revealed a cardiac mass that was 3 cm in maximum diameter; the mass was removed and confirmed as cardiac myxoma by pathology evaluation. She recovered from motor weakness, but lost vision in her right eye due to this event.
By using cerebral angiography, multiple cerebral aneurysms were identified (Fig. 1). Among them, a right MCA fusiform aneurysm was the largest, with a diameter of 19.5 mm; it had developed at the site of the previous MCA occlusion. Considering the risk of rupture, surgery was planned with preparation for superficial temporal artery-MCA bypass. During surgical exploration, the MCA aneurysm, which had been suspected as a fusiform aneurysm, was identified as an MCA bifurcation aneurysm with permanently occluded inferior trunk toward the temporal lobe. The aneurysm exhibited a rubber-like feature; notably, a feasible resolution was M2-M2 end-to-end anastomosis with resection of aneurysm (Fig. 2). Anastomosis was successfully performed, and biopsy showed dilation and thickening of the aneurysmal wall without any evidence of tumor invasion.

(A) Right internal carotid artery digital subtraction angiography showing right middle cerebral artery (M1 segment) occlusion. (B) Reperfusion via right middle cerebral artery after intravenous tissue-type plasminogen activator injection. (C, D) Right internal carotid artery digital subtraction angiography anteroposterior and lateral views showing multiple aneurysms. (E) Right middle cerebral artery bifurcation aneurysm was 19.5 mm in maximum diameter on 3-dimensional reconstruction image. (F) T2-weighted magnetic resonance image showing large aneurysm at the right middle cerebral artery.
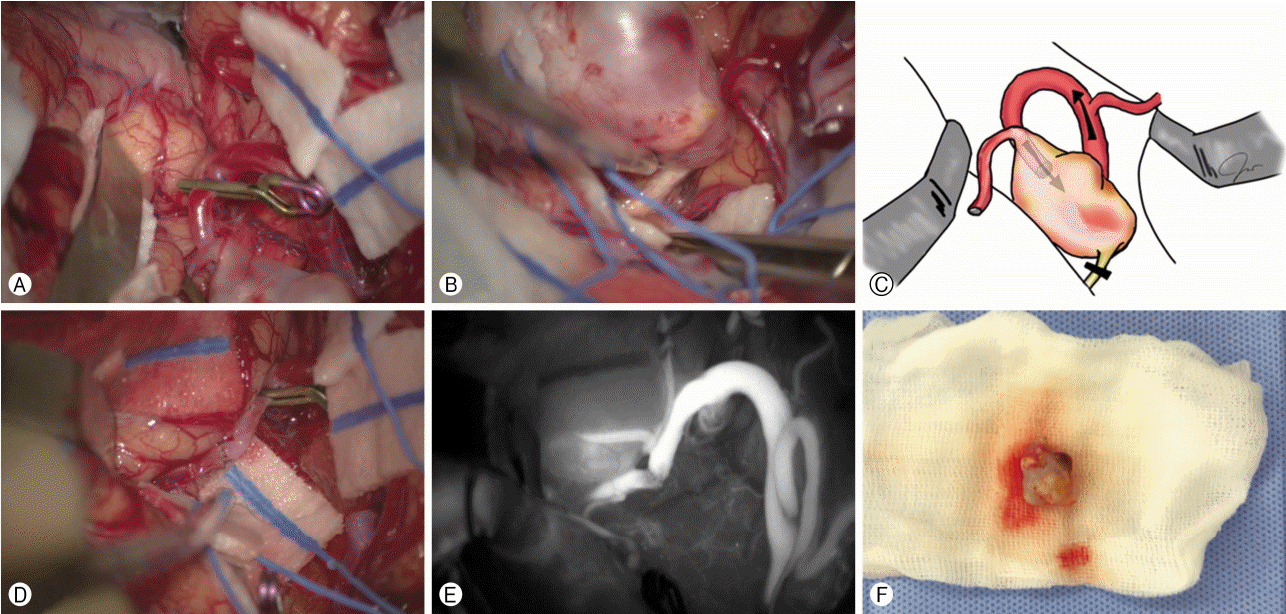
(A–C) Bifurcated middle cerebral artery aneurysm with permanently occluded inferior trunk toward temporal lobe was observed during surgical exploration. (D, E) M2-M2 end-to-end anastomosis with resection of aneurysm was successfully performed. (F) Biopsy showed dilation and thickening of the aneurysmal wall.
DISCUSSION
Cardiac myxoma is the most common primary heart neoplasm, constituting 50% of all cardiac tumors; its incidence is approximately 0.5 cases per 1,000,000 population per year1). There are two main types. Most myxomas are smooth, firm masses that can be calcified or ossified. A small proportion of myxomas are soft, gelatinous tumors with irregular fronds; these often embolize. Although they are benign tumors with a classical risk of metastasis, such embolization can cause ischemic events or aneurysms4).
Neurologic complications associated with cardiac myxoma are observed in up to 35% of patients6). In the literature, symptoms of stroke or peripheral ischemia due to embolization are reported in approximately 22% of myxoma cases. The incidence of embolization is not related to the size of the tumor, but is instead related to tumor mobility and friability1,10).
Myxomatous aneurysms, intracranial aneurysms associated with cardiac myxoma, are less common; their true incidence is unknown, but reports of such aneurysms are increasing with improvements in cardiac and neurovascular imaging that facilitate early detection of disease8). The mechanism for the formation of intracranial aneurysms in conjunction with cardiac myxomas is not well-established, but some hypotheses have been proposed: (1) Myxomatous emboli can block the vasa vasorum, destroying the normal architecture of the vessel, similar to mechanism of mycotic aneurysms; the vessel wall becomes vulnerable to ischemic injury and subsequent dilatation, which lead to aneurysm formation2,8); (2) Myxomatous emboli produce vascular occlusion, causing scarring and pseudoaneurysm formation; (3) Tumor cells can proliferate and penetrate the wall; either mechanism can lead to scarring of the vessel wall and pseudoaneurysm formation11,13). The angiographic characteristics of myxomatous aneurysms are multiplicity, fusiform appearance, and distal location. These features are similar to those of immunodeficiency-associated aneurysms and septic emboli-causing aneurysms5,7,16).
Treatment options for myxomatous aneurysms are conservative care, endovascular methods, or surgery. These aneurysms may remain stable for many years; additionally, spontaneous regression of intracranial myxomatous aneurysms has been frequently reported9,12,14). Therefore, without a specific risk factor, conservative treatment with serial MR imaging or angiography follow-up can be a reasonable strategy, especially when the risk of surgical treatment is high15). Cases of ruptured aneurysm are generally considered urgent surgical candidates. Because of the fusiform shape of most myxomatous aneurysms, it is difficult to perform conventional clipping of the aneurysm while maintaining the flow of the parent artery; bypass surgery is a reasonable option when sacrifice of the feeding artery may be required. In this case, M2-M2 end-to-end anastomosis was performed with complete resection of the myxomatous aneurysm. However, bypass surgery is technically challenging, compared with other options, and is limited because it is difficult to apply in a variety of locations. Additional case studies are needed regarding the location of myxomatous aneurysms and successful surgical approaches. Endovascular treatment is a reasonable treatment option. Because of the fusiform shape, coil embolization with stenting could be necessary7). There remains much debate regarding the possibility that chemotherapeutics can stabilize myxomatous aneurysms when surgery or endovascular procedure is not possible3).
In conclusion, our case shows that surgical resection with bypass surgery is a useful option for the treatment of cerebral myxomatous aneurysms.
Notes
No potential conflict of interest relevant to this article was reported.