Paresthesia and Pain in Both Arms when Shampooing One’s Hair: Symptoms of Neurogenic Thoracic Outlet Syndrome
Article information
Abstract
Neurogenic thoracic outlet syndrome (TOS) is a clinical diagnosis based on the reproduction of a patient’s symptoms with a provocation test (arm elevation) after excluding other conditions that might cause similar symptoms. Neurologic symptoms and signs can vary from mild paresthesia and numbness to intrinsic hand muscle atrophy. The main controversy in patients with neurogenic TOS involves neurologic-type complaints of paresthesia, numbness, and pain. However, there is no positive objective test to identify the cause. A 54-year-old female patient presented with numbness and radiating pain in her bilateral arms that occurred every time she bowed her head while shampooing. The patient had a history of two neck sprains due to slipping before the onset of symptoms. In addition to pain and numbness in both arms at arm elevation, pain in the suprascapular and occipital areas was also present. After excluding cervical nerve root lesions and other bone abnormalities, the patient's symptoms disappeared by brachial plexus decompression through a supraclavicular approach. It is difficult to diagnose neurogenic TOS with pain and paresthesia without muscle weakness in the upper extremities. If physicians do not consider the possibility of neurogenic TOS in patients with upper extremity paresthesia and pain, unnecessary multiple treatments may be performed, prolonging patients’ suffering. The exacerbation of pain and paresthesia in both arms and hands can occur immediately after the head is lowered during shampooing. This can be interpreted as a characteristic symptom of a constricted interscalene triangle and brachial plexus compression caused by hyperabduction of the arm.
INTRODUCTION
Thoracic outlet syndrome (TOS) refers to compression of the subclavian vessels and brachial plexus in the region of the superior aperture of the chest, with the most common compression of these structures against the first rib8). Historically, the diagnosis and treatment of TOS have been difficult and controversial topics4,8). For example, even the term of the thoracic outlet is confusing8). Anatomically, the area between the scalene muscles and the first rib is termed the thoracic inlet13). Neurologic symptoms and signs can range from mild paresthesia and numbness to intrinsic hand muscle atrophy4,9). In many cases, there might be concomitant distal peripheral nerve entrapment such as cubital or carpal tunnel syndrome8). In neurogenic TOS, there is no reliable objective test to identify the cause. Nerve conduction studies (NCS) are useful for detecting sites of concomitant distal nerve compression, such as the median nerve at the carpal tunnel and the ulnar nerve at the elbow4,8,9). However, neither NCS nor somatosensory-evoked potentials (SSEPs) are universally accepted as helpful in diagnosing neurogenic TOS4,8,9). In these cases, the diagnosis of TOS is suggested by physical examination and provocative test4,8,9).
We want to report a very rare case of paresthesia accompanying arm elevation. It occurred on both arms as the main symptom whenever the head was bowed. A hyperabduction test of the arm on physical examination was helpful for the diagnosis. Subsequent decompression of the brachial plexus via the supraclavicular approach successfully relieved the pain and paresthesia of the neurogenic TOS.
CASE REPORT
A 54-year-old female patient presented with numbness and radiating pain in her bilateral arms every time she bowed (Fig. 1A). The patient slipped and fell two years ago, suffered neck pain, and underwent an anterior C5/6 cervical fusion surgery a month later. Her neck pain disappeared after the surgery. A year before her visit, she fell backward while sitting in a wheelchair with a cast on her foot due to an ankle sprain. Her back and right shoulder hit the ground, although no pain occurred. Three months later she fell backward again. From then on, she developed numbness and pain in her neck, shoulders and arms. When the patient stayed still, there was no pain. However, when the patient lowered her head, a momentary numbness occurred in both arms. The numbness in both arms and pain in the neck and shoulders occurred every time the patient bowed her head. There was no numbness when the patient moved her arms or shoulders.
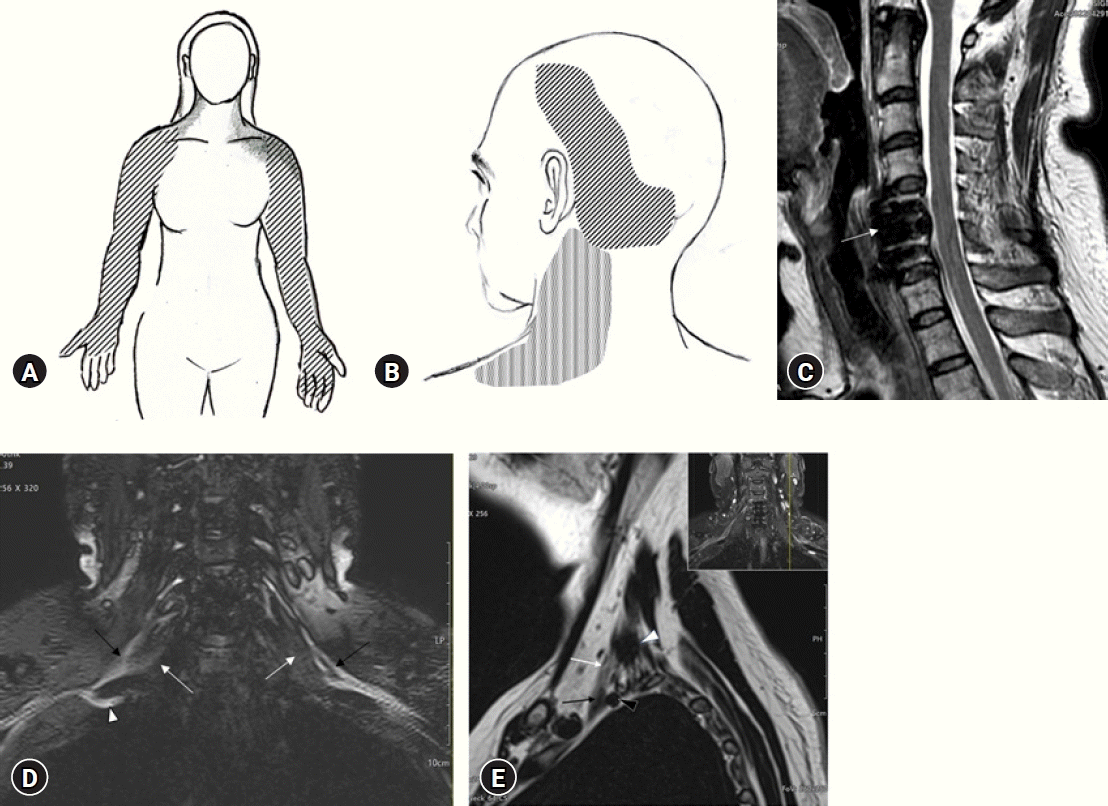
Distribution of bilateral arm pain and radiologic findings. (A) Distribution of pain and paresthesia (hatched area) in the bilateral arms and hands. The gray area indicates the distribution of the aching pain associated with arm paresthesia. (B) Distribution of aching and tightening pain in the left occipital area. It radiated to the temporoparietal vertex and posterolateral neck. (C) Sagittal T2-weighted magnetic resonance imaging of the cervical spine showing no abnormality, except for prior C5/6 anterior cervical discectomy fusion (arrow). (D) A coronal T2-weighted, enhanced, short tau inversion recovery image of the brachial plexus showing suspected hypertrophy of the anterior scalene muscle (white arrows) and interdigitation of the contour of the brachial plexus (black arrows). Deviation in the course of the lower trunk of the right brachial plexus (white arrow) was noted. (E) A sagittal T2-weighted image of the left brachial plexus shows the left brachial plexus (white arrow) leaving the interscalene triangle between the anterior (black arrow) and middle (white arrowhead) scalene muscles. The back arrowhead indicates the subclavian artery.
In the early stages of pain, the pain that occurred momentarily disappeared immediately. Over time, the duration of pain and numbness accompanied by lowering the head increased. Sometimes, as the momentary pain lasted for more than 5 min, the patient had no choice but to stay still while waiting for the pain to go away. Sometimes numbness occurred in both arms and left upper back when the patient turned her head sideways. At night, numbness occurred in the arms according to the posture of the neck. Six months prior to her presentation, the pain intensified, making the patient's daily life difficult. In particular, when the patient bowed her head while shampooing, the pain in both arms lasted for more than two hours. Along with numbness in both arms when bowing the head, a tightening pain occurred in the left occipital area. Occipital pain was tightening and squeezing in nature. It lasted all day. It radiated to the left temporal and posterolateral neck (Fig. 1B). She was treated at a hospital where she underwent cervical surgery. She was told that there was no problem with the cervical spine surgery site and that there was no additional cervical disc herniation (Fig. 1C). Drug treatment and physical therapy were performed for 6 months. However, there was no improvement in symptoms. The occipital pain did not improve with nonsteroidal anti-inflammatory drugs (NSAIDs), including Ultracet®, gabapentin, pregabalin, muscle relaxants, and occipital nerve blocks.
On physical examination, no specific findings were observed except for the surgical scar for cervical fusion on the front neck. It was confirmed that immediate numbness occurred in both arms when the patient bowed her head. Numbness in both arms occurred even when the patient's head was turned to the side a lot. However, limitation of neck motion was not confirmed. Neurological examination revealed that both arms and hands had no motor weakness. Pinch and grip strengths were also found to be normal. The deep tendon reflex was normoactive. Mild hypesthesia was observed in the left supraclavicular region, shoulder, and upper lateral region of the left upper arm. A slight tenderness was found in the left supraclavicular region. However, no paresthesia was induced upon compression.
Percussion of the nerve (Tinel’s sign) was negative in the common nerve entrapment site (carpal tunnel, median nerve forearm, cubital tunnel, and brachial plexus) of the upper extremity. However, hyperabduction of bilateral arm to 180 degrees while keeping wrists and elbows straight for 1 min produced mild paresthesia of bilateral arms and hands, and it was judged to be positive. The Wright hyperabduction and Adson tests were negative. The Spurling’s test was also negative. There were no systemic diseases to cause pain. Laboratory findings showed no abnormalities. Electrodiagnostic tests including electromyography (EMG), nerve conduction test, and SSEP was all normal. Plain radiographs of the chest and cervical spine showed no cervical ribs or other bony abnormalities such as prominent transverse process or old clavicle fractures, or findings of degenerative arthritis, such as instability, osteophytes, or intervertebral disk space narrowing other than C5/6 anterior cervical fusion. Computed tomography (CT) and magnetic resonance imaging (MRI) of the cervical spine showed no evidence of residual stenosis or adjacent segment degeneration after cervical surgery. Hypertrophy of scalene muscles and irregularity of the brachial plexus contour was suspected on brachial plexus MRI (Fig. 1D). Decompression of the brachial plexus was proposed with a possibility of brachial plexus entrapment (i.e., neurogenic TOS) and medical intractability in mind.
The supraclavicular approach for decompression of the brachial plexus was performed first on the left side, where the pain was more severe. The operation was performed under general anesthesia and intraoperative neurophysiological monitoring according to the method suggested by Mackinnon et al.1,2,4). The patient was supine with an underlying shoulder pump to extend the neck. After making an 8-cm linear skin incision about two centimeters above and paralleling the clavicle, supraclavicular nerves were identified and protected deep to the platysma muscle. Dissection was carried down by dividing the omohyoid muscles, elevating supraclavicular fat pad, and partially dividing the sternocleidomastoideus muscle. After securing the phrenic nerve in front of the anterior scalene muscle in the field of view, it was found that the upper trunk of the left brachial plexus was compressed and swollen between anterior and middle scalene muscles (Fig. 2A). The anterior scalene muscle was divided, taking care not to injure the phrenic nerve with bipolar cautery. Division of the anterior scalene muscle led to exposure of the middle trunk. The long thoracic nerve was isolated from the lateral and posterior part of the middle scalene muscle. Whether shoulder contraction was induced by intraoperative electrical stimulation was then checked. The middle scalene muscle inserted into the first rib was then divided to expose the lower trunk of the brachial plexus. All tendinous edges of scalene muscles around the plexus and fibrous sheath of the nerve, which could potentially entrap the nerve, were removed from view under a microscope (Fig. 2B). After securing hemostasis and applying an anti-adhesion gel and films, the overlying wound was closed in layers with closed suction drainage left in the wound. The postoperative course was uneventful. Gentle range of neck motion started with active ambulation permitted within two days after surgery.

Intraoperative photographic findings of neurogenic thoracic outlet syndrome during decompression surgery via the supraclavicular approach. (A) An intraoperative photograph showing the upper trunk (black arrows) of the left brachial plexus. The upper trunk was found to be impinged between the anterior (white arrows) and middle (white arrowhead) scalene muscles. The white star indicates the left phrenic nerve, branching from the upper trunk. (B) An intraoperative photograph showing decompression of the left brachial plexus. Indentation and distortion of the course of middle and lower trunks of the brachial plexus medial to the upper trunk (black arrows) were found between cut edges of the anterior (white arrow) and middle (white arrowhead) scalene muscles. The white star indicates the left phrenic nerve. The black arrowhead indicates the long thoracic nerve. (C) An intraoperative photograph showing the upper trunk (black arrows) of the right brachial plexus. The upper trunk was swollen and fixed between the tense anterior (white arrows) and posterior (white arrowhead) scalene muscles. The white star indicates the left phrenic nerve overlying the anterior scalene muscle. (D) An intraoperative photograph showing completed decompression of the right brachial plexus (black arrows). Indentations of the lower and middle trunks of the right brachial plexus were observed medial to the upper trunks (black arrows) between cut edges of the anterior (white arrow) and middle (white arrowhead) scalene muscles. The long thoracic nerve (black arrowhead) was isolated from the middle scalene muscle.
In an interview two weeks after the surgery, no neurological abnormalities were observed in the left arm. The pain in the surgical site was minimal. The patient reported that the numbness in the left arm when the head was bowed no longer occurred, although it was still present in the right arm. The pain in the left occipital area along with the pain in the left arm completely disappeared. The patient requested an expedited surgical schedule for her right arm pain.
Decompression of the right brachial plexus was performed one and a half months after the operation on the left. It was performed in the same manner as in the first left surgery (Fig. 2C, D). The patient was discharged on the 5th day after surgery. After a month, it was confirmed that the numbness and pain in the right arm that had occurred when the patient bowed his head also disappeared. However, weakness was found in the abduction of the right shoulder. The largest abduction angle of the shoulder was only possible to 90 degrees. There were no restrictions on right shoulder flexion, extension, or adduction. No sensory disturbance or pain was identified. Abduction paralysis of the right shoulder improved to 120 degrees 3 months after the operation. It was no longer observed at six months. Twelve months after the operation, the patient's arm numbness due to neck flexion no longer occurred. There was no disturbance in daily life.
DISCUSSION
1. Neurogenic TOS
TOS is a constellation of clinical manifestations in the neck, shoulder, and upper extremities caused by compression of neurovascular structures in the thoracic outlet region1,2,4). Its debated history, pathophysiology, and even existence make TOS the most controversial topic in peripheral nerve surgery4). The lack of professional consensus, in combination with a wide variability of symptoms and lack of a gold standard for its diagnosis, can explain how a diagnosis for a patient with this condition is often overlooked4). In this context, it took more than a year for the numbness of the arm accompanying head bending in the current case to be diagnosed as neurogenic TOS. Thus, its diagnosis is difficult if a patient is not observed or examined with TOS in mind. Some experienced researchers have emphasized general principles of the cause and symptoms of TOS4). They believe that paresthesia and numbness experienced in hand with overhead activities are related to compression of the brachial plexus while the frequently more concerning problem of pain in the scapular, neck, and shoulder is related to muscle imbalance4). In this context, we could suspect TOS in the current case based on the fact that hair shampooing as an overhead activity exacerbated the numbness for more than two hours. However, in order to diagnose it, some processes were required to exclude other structural causes.
Neurogenic TOS is thought to result from a combination of a congenial anatomical predisposition and trauma to the neck3,4,15). Another common cause is a poor posture of the neck, upper back, and shoulders4). Obesity and a propensity for increased flexion of the neck and shoulders have been suggested as factors that increase the incidence of neurogenic TOS4).
TOS typically occurs in young and middle-aged adults. It occurs in women three times more frequently than in man2). Patient symptoms may differ depending on which structure is compressed in the cervicoaxillary canal4). The subclavian vein, the subclavian artery, and the brachial plexus are three neurovascular elements involved in TOS. That is, symptoms of nerve compression are different from those of arterial or venous compression. Neurogenic TOS is much more common than arterial or venous TOS, accounting for up to 98% of cases2,4). Arterial TOS has symptoms such as cold extremities, easy fatigue, and Raynaud syndrome caused by ischemia in the upper extremity. Venous TOS is mostly related to axillary subclavian vein thrombosis4). Therefore, neurogenic TOS presented as numbness and pain in the upper extremity can be distinguished easily from vascular TOS based on symptoms. Although neurogenic TOS is more common than vascular TOS, it is typically more difficult to diagnose neurogenic TOS because its greater variability in symptomatology. Fifteen percent of cases might have some concomitant arterial symptoms. However, arterial symptoms seldom exist alone4). Physicians who diagnose only vascular forms of TOS are misdiagnosing the vast majority of patients they see who have neurologic TOS4).
2. Anatomy of TOS
The brachial plexus has a course between the anterior and middle scalene muscles. It continues distal deep to the clavicle and superior to the first rib. This opening is anatomically referred to as the thoracic inlet and clinically as the thoracic outlet8,13). Three different compartments in the cervicoaxillary canal are related to the genesis of neurovascular compression syndrome: the interscalene triangle, the costoclavicular space, and the pectoralis minor region4-7,11). The medial or proximal segment of the cervicoaxillary canal comprises the scalene triangle and costoclavicular space, where the majority of neurovascular compression occurs4).
The anterior scalene muscle originates from the anterior tubercles of the transverse processes of the third through sixth cervical vertebrae. It inserts onto the scalene tubercle of the first rib. The middle scalene originates from the posterior tubercles of transverse processes of the second through seventh cervical vertebrae. It inserts onto a more posterior portion of the first rib. The subclavian artery and the brachial plexus pass through the space posterior to the anterior scalene muscle called scalene triangle or interscalene space. This space is bounded by the anterior scalene muscle anteriorly, the middle scalene muscle posteriorly, and the first rib inferiorly. It has some overlap with the posterior space of the costoclavicular space4). It has been acknowledged that significant distortions of the cervicoaxillary canal and its neurovascular contents can occur due to a wide range of shoulder and upper extremity motions4). The brachial plexus and subclavian artery become compressed when the scalene triangle is narrowed with hyperabduction of the arm4). When the superior aspect of the scalene triangle is narrowed, the upper components of the brachial plexus become compressed. When the floor of the triangle is elevated, the lower components of the brachial plexus and the subclavian artery become compressed4).
3. Diagnosis of Neurogenic TOS
The diagnosis of TOS is based on findings of clinical evaluation, particularly if symptoms can be reproduced when various dynamic maneuvers including elevation of the arm are undertaken3,9). Therefore, clinical diagnosis of TOS is often difficult. Imaging tests such as CT and MRI that can confirm anatomical structures of the thoracic outlet are essential along with EMG4,8,9).
The onset of symptoms of TOS may be insidious or follow trauma4). Neck and shoulder pain and stiffness might be early signs of muscle spasm and imbalance4,8). Pain and paresthesia associated with nerve dysfunction are present in up to 95% of cases. They typically occur in delayed fashion weeks or months later, often after acute musculoskeletal symptoms have resolved3,4). Numbness may present with or without tingling. Symptoms might be exacerbated following strenuous physical activity or prolonged arm elevation4). The occurrence of symptoms after activity can help us distinguish TOS from primary shoulder or cervical spine pathology when symptoms tend to occur during activity4). Symptoms of neurogenic TOS depend on which trunk of the brachial plexus is involved4). The lower trunk is known to be most commonly involved4). When isolated upper trunk symptoms occur, cervical spine pathology is often the causative agent4). When the upper trunk is involved in TOS, symptoms occur in the neck, deltoid area, and lateral ar. They may also radiate to the side of the face, the ear, the occiput, and in the median nerve distribution4,8,9).
It is important to distinguish between the more common cervical spine diseases and TOS4). Common cervical spine diseases such as cervical disk disease and spondylosis causing nerve root compression are usually associated with neck pain, stiffness, radiating paresthesia, and weakness of involved cervical roots4). Generally, they are common in the C5-C6 or C6-C7 intervals, creating symptoms in the respective nerve root distribution. Because the lower trunk of the brachial plexus is most commonly involved in TOS, compression of the C8 or T1 nerve roots can more closely mimic TOS, with symptoms in an ulnar nerve distribution. However, cervical disk disease involving the C8 or T1 is much less common than compression of the fifth, sixth, or seventh roots4).
Among several provocative maneuvers of neurogenic TOS, hyperabduction test described by Novak et al.10,11) was positive in the current case. However, other physical tests such as the wright hyperabduction test, Adson test, Halstead test, and costoclavicular test were negative. Flexion of the neck typically induced characteristic pain and paresthesia in bilateral arm in the current patient. Hair shampooing as an overhead activity characteristically exacerbated arm numbness for several hours. Narrowing of the scalene triangle due to hyperabduction of the arm is well acknowledged. At the same time, neck flexion was thought to increase the tension of hypertrophied anterior and middle scalene muscles, resulting in increased compression of the brachial plexus. In addition, overhead activities of bending the neck and raising the arms during hair shampooing are interpreted as conditions that can cause a narrowing of the cervical axillary canal, especially the scalene triangle.
Imaging tests such as CT and MRI are needed to investigate congenital or other organic causes of TOS such as tumors or other space-occupying soft tissue lesions9). Generally, these studies are not necessary for patients with TOS9). However, they may help us rule out the presence of cervical disk disease, spinal stenosis, or nerve root impingement5-7). Both MRI and ultrasound are thought to be useful when performed with provocative maneuvers such as hyperabduction of the arm. They can detect vascular TOS to a greater degree than detecting neurogenic TOS5-7). Therefore, unlike vascular TOS, imaging-based diagnosis has limitations in neurogenic TOS4).
CT and MRI might be helpful in the identification of soft tissue abnormalities associated with TOS. Several anatomical variations of the scalene muscles have been suggested to be responsible for TOS7). They include hypertrophy of the anterior scalene muscle, origin of the anterior and middle scalene muscles from a common belly that divides in two distally, the passage of the brachial plexus through the substance of the anterior scalene muscle, a broad middle scalene muscle inserting more anteriorly on the first rib than what is normal, interdigitation between the anterior and middle scalene muscles, supernumerary muscle such as scalenus minimus muscle, and anomalous fibrous bands5-7,12,14,17). However, the clinical significance of these findings in TOS remains unclear.
Electrodiagnostic studies are typically normal in patients with TOS unless TOS is associated with cubital or carpal tunnel syndrome4). NCSs and EMG are controversial in diagnosing TOS4,8,9). They are helpful for identifying more peripheral nerve compression that may exist with TOS concomitantly2). EMG findings tend to become positive only late in pathology4). NCSs, especially ulnar nerve conduction velocities, have been suggested to be more useful for the earlier detection of TOS13). However, some authors remain pessimistic about its usefulness4,8,9).
4. Management of Neurogenic TOS
It is known that 50% to 80% of patients with neurogenic TOS improve through physioptherapy10). The main goal of physical therapy is to decrease external nerve compression resulting from muscle imbalance4,9). Stretching and strengthening exercises focus on correcting abnormal posture while restoring muscle balance4,9). If TOS symptoms do not improve with physiotherapy, the release of any concomitant distal nerve compression such as a cubital tunnel or carpal tunnel syndrome is recommended4,9). Although the risk of surgical decompression of thoracic outlet by skilled operators is very low, surgery should be selected with caution due to the potential of serious morbidity of high nerve injury4,9). If there are no cervical ribs, decompression of the brachial plexus via scalenotomy is recommended4,9). Generally, first rib resection is recommended when there is a significant compressive element17).
For thoracic outlet decompression, several surgical approaches have been proposed, including high posterior thoracoplasty, anterior approach, and transaxillary approach4,8,9). Scalenotomy alone is associated with a higher long-term recurrence rate of up to 65%4,8,9). We adopted the supraclvacular approach for the brachial plexus decompression suggested by Mackinnon et al.8) It allows surgeons complete visualization of all the neurovascular elements and removal of the first rib4). During dissection, care should be taken to preserve the supraclavicular and long thoracic nerves. Gentle but early postoperative movement of the head, neck, and upper extremity is encouraged to minimize scar formation around the brachial plexus8). For neurogenic TOS, first rib resection is not necessary for satisfactory relief of symptoms4,8). In the present case, there was no bone pathology like a cervical rib. Sufficient decompression of the brachial plexus was possible without first rib resection. Intraoperative nerve stimulation was helpful for identifying the long thoracic nerve during dissection of the middle scalene muscle. Surgical failure and recurrence are known to be relatively common2). Repeated decompression is warranted for appropriately selected patients16). In case of reoperation, an alternative approach such as the posterior thoracoplasty approach is recommended to reduce dissection in a previously scarred bed and consequent risk of nerve or vessel injury8,9).
CONCLUSION
Diagnosis and treatment of TOS remain controversial and difficult, particularly in patients with neurogenic TOS without muscle atrophy. In these patients, the diagnosis of neurogenic TOS can be made by provocative testing after excluding other potentially causative conditions. Most patients improve with conservative management, including activity, posture modification, and physical therapy. Those with persistent significant symptoms are candidates for surgical decompression with a supraclavicular approach.
Notes
No potential conflict of interest relevant to this article was reported.