Aneurysmal Subarachnoid Hemorrhage in Young Adult Patients: Single Center Reports
Article information
Abstract
Objective
The mechanisms underlying the formation and rupture of intracranial aneurysms in young adults remain a matter of debate. This study aimed to evaluate the clinical characteristics of young adult patients with aneurysmal subarachnoid hemorrhage (SAH) treated with endovascular or clipping techniques at a single center.
Methods
Seventeen young adult patients (age, 18–40 years; 7 men and 10 women; mean age, 35.7 years) with aneurysmal SAH were treated at our hospital using an endovascular or clip ligation approach between February 2018 and March 2023. The clinical outcomes, complications, and patient characteristics were evaluated. The mean follow-up duration was 13 months (range, 0–44 months).
Results
The male-to-female ratio was 0.7 (7 vs. 10 patients), and the most common location of aneurysm was the internal carotid artery (7 patients, 41.2%). Two patients (11.8%) presented with a history of hypertension, and six (35.3%) with smoking. The overall favorable outcome rate was 64.7% (Glasgow Outcome Scale [GOS] 4 and 5), while unfavorable outcomes occurred in 35.3% of patients (GOS 1, 2, and 3). None of the patients rebounded after clipping or endovascular treatment. Two (14.3%) patients treated with coil embolization (14 patients) showed an interval change in the residual neck (recanalization).
Conclusion
Our results suggest that young adults with ruptured intracranial aneurysms exhibit different characteristics. However, well-controlled investigations using larger prospective studies are warranted to further clarify the clinical characteristics of these patients, including the mechanisms of aneurysm formation and rupture.
INTRODUCTION
Intracranial aneurysms, both ruptured and unruptured, mostly occur in patients over 40 years. Aneurysmal subarachnoid hemorrhage (SAH) is uncommon in patients aged <40 years (10%–20% of intracranial aneurysms)1,6,9,11,15,21). However, its incidence in young adults has recently increased. This tendency has led to the belief that intracranial aneurysms are not congenital but acquired, and that hemodynamic stress may serve as a major factor in aneurysm formation and rupture6,9,15). Despite extensive literature discussing cerebral aneurysms in the general population, there remains a paucity of data pertaining specifically to the occurrence, clinical features, management, and outcomes of intracranial aneurysms in young adult patients.
MATERIALS AND METHODS
We retrospectively reviewed the medical records of young adult patients (aged 20–40 years) with aneurysmal SAH between February 2018 and March 2023. The total number of patients with aneurysmal SAH during the study period was 246. Seventeen (6.9%) young adult patients with aneurysmal SAHs were treated at our hospital using endovascular or clip ligation (craniotomy). The selection criteria for this study were age between 20 and 40 years at the time of surgery; endovascular or clip ligation approach chosen as treatment; and exclusion of patients with fusiform, traumatic, or mycotic aneurysms. All patients were diagnosed using computed tomography and underwent conventional angiography of the carotid and vertebral arteries.
We analyzed patients according to several characteristics. Clinical characteristics included Hunt-Hess grade, Fisher grade, and Glasgow Outcome Scale (GOS) score. The aneurysm characteristics included location and size. We also reviewed the risk factors (hypertension and smoking) and perioperative complications (aneurysm rupture, hydrocephalus, and vasospasm).
RESULTS
1. Patients Characteristics
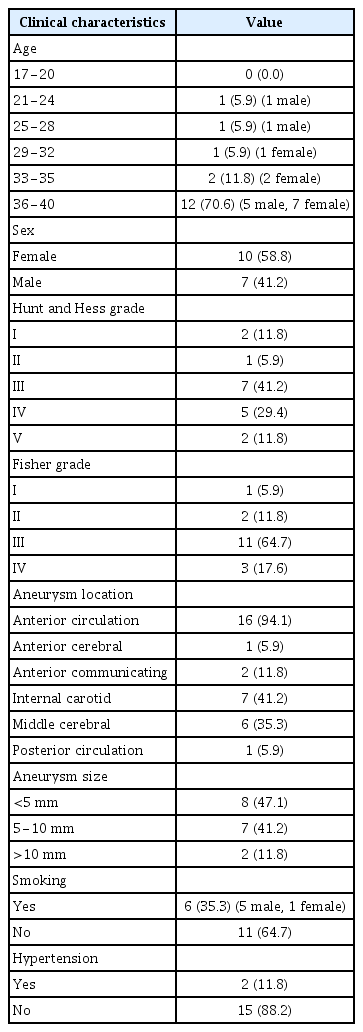
The total number of young adults with SAH was 20. One traumatic, one non-aneurysmal, and one SAH originating from an arteriovenous malformation were excluded. We selected 17 patients whose age was between 20 to 40 years old, and this group comprised 7 men (41.2%) and 10 women (58.8%), with a mean age of 35.7 years (range, 22–40 years). Two patients (11.8%) had hypertension and six (35.3%) had a history of smoking (Table 1).
2. Clinical Characteristics
At admission, patients with good grade (Hunt & Hess grades I [2 patients], II [1 patient], and III [seven patients]) were 58.8%, and those with bad grade (Hunt & Hess grades IV [5 patients] and V [2 patients]) were 41.2% (Table 1).
3. Aneurysm Characteristics
Our study includes sixteen anterior circulation aneurysms (94.1%) and 1 posterior circulation aneurysm (5.9%). The internal cerebral artery (7 patients, 41.2%) was the most frequent aneurysm site. Multiple aneurysms included of our study were seen in three patients (17.6%). Eight small (<5 mm), seven medium (5–10 mm), and two large (>10 mm) aneurysms were observed (Table 1).
4. Clinical Outcomes and Complications
After treatment, patients with favorable outcomes (GOS 4 [9 patients], and 5 [2 patients]) comprised 64.7%, and those with unfavorable outcomes (GOS 3 [2 patients], and 2 [1 patient] and 1 [3 patients who died of massive brain edema]) comprised 35.3%. None of the patients rebounded after clip ligation or endovascular treatment. Two patients who showed signs of acute hydrocephalus underwent external ventricular drain, and eventually required ventriculoperitoneal shunt insertion (Table 2).
5. Endovascular Results
Fourteen endovascular treatments were performed (82.4%), which resulted in eight complete obliterations with no contrast filling of the aneurysmal sac (57.1%), six small residual neck (42.9%) with no residual delayed contrast stagnation of the aneurysmal sac (Table 2), and three patients died. Plain skull imaging follow-up (mean follow-up duration, 14 months; range, 2–41 months) was performed for all 11 surviving patients. Five patients (35.7%) showed interval changes in the residual neck (recanalization of aneurysmal sac). Two patients required further treatments.
6. Results of surgical Treatment
Three craniotomy and aneurysm clipping operations were performed (17.6%) (Table 2). They included two middle cerebral artery (MCA) aneurysms (11.8%) and one ACoA aneurysm (5.9%). All surgical treatments resulted in a complete obliteration. A follow-up with magnetic resonance angiography and transfemoral cerebral angiography was performed (mean follow-up duration, 15.3 months; range, 6-28 months). None of the patients required further treatments.
DISCUSSION
1. Sex Distribution
According to previous studies7,10,15), sex differences exist in the prevalence of aneurysmal SAH in young adults. Several large center studies have shown female dominance. The ratio increased with age in every decade. Our study demonstrated a female-to-male ratio of 1.4:1 predominance of women. This result was consistent with the findings of previous studies7,9,10,13,15).
2. Location of Aneurysm
Previous studies have demonstrated differences in the location of intracranial aneurysms between young adult and adult patients, and intracranial aneurysms in young adults are generally reported to develop in the internal carotid artery (ICA) or anterior cerebral artery (ACA). The incidence of MCA aneurysms in young adults is low3,7,9,10,13). Most aneurysms in our study were located in the circle of Willis in the anterior circulation, particularly in the ICA. The results of a previous study are compatible with ours. Ogungbo et al.13) showed that 93.9% of anterior circulation aneurysms rupture, and the occurrence of ICA aneurysm was 35.7% (our results were 94.1% and 41.1%, respectively).
Previous authors have postulated that younger patients tend to have more proximal aneurysms involving the ICA as opposed to older patients, who have an increased incidence of ACA aneurysms3,7,10,13). A previously suggested hypothesis argues that this difference stems from an embryological process in which the ICA develops before the ACA and MCA; therefore, hemodynamic stress causes a defect in a congenitally fragile ICA earlier than in the ACA 2). Thus, a fragile and congenital portion of the ICA may develop into an aneurysm owing to hemodynamic stress, and the development of an ACA aneurysm may take longer than the growth of an ICA lesion7). There were some differences in aneurysm locations between males and females. In males, ruptured aneurysms were more common in the ACA, whereas in females, the ICA location was more frequent3,7,15,18).
3. Contributing Risk Factors
Intracranial aneurysm formation and rupture are associated with older age, female sex, and smoking13). Aneurysmal SAH is rare in patients aged <40 years old. Young patients account for 5% to 17% of the SAH population1,7,9-11,13-15).
Smoking is thought to influence the incidence of SAH in young adults2,4,5,8,12,16,17,22,23). Thirty-five percent of our patients were active smokers versus 20.8% of the United States adult population20). The increased incidence of aneurysms with age in women is associated with various factors. Such factors, most notably smoking and menopause, influence the development of aneurysms. The importance of endogenous and exogenous hormonal factors demonstrates the possible reduction in SAH in premenopausal women, particularly in those with no history of smoking. Furthermore, hormone replacement therapy was found to reduce the risk of SAH in postmenopausal women who had never smoked10,13,16,17,22,23). Usually, young adults do not exhibit hypertension or atherosclerosis. Clinically and radiologically, no factors could be found in young adults that increased hemodynamic stress sufficiently to contribute to aneurysm formation9). Hypertension is not always present in patients with aneurysms, and other obscure factors play a role in lesion formation13).
4. Mechanism for Formation and Rupture of Aneurysms in Young Adults
However, the mechanisms underlying the formation and rupture of intracranial aneurysms remain unclear. Documented instances of familial aneurysms in some populations and the role of genetics in aneurysm formation have been previously reported. Pathologically, the aneurysmal walls in young adults show alterations similar to those in adults, such as medial defects and interrupted internal elastic laminae. Degeneration of the internal elastic lamina appears to be essential for aneurysm formation, and atherosclerosis is regarded as a major factor in such degeneration and is also generated by hemodynamic stress augmented by hypertension. The vast majority of ruptured aneurysms in young adults occur in the anterior circulation, particularly the ICA. The ICA has a greater blood flow than the anterior communicating and middle cerebral arteries, which may exert intense hemodynamic stress on the arterial walls. Hemodynamic forces are believed to be responsible for aneurysm rupture in older adults. Vessel wall damage caused by atheroma and increased stress caused by hypertensive circulation predispose aneurysms to rupture7,9,10,13,15,19,23). The formation and rupture of aneurysms seem to depend on the imbalance between arterial durability and hemodynamic stress. Such arterial fragility may reduce durability and is related to aneurysm formation and rupture, resulting in a remarkably fragile aneurysmal wall. Some authors have stressed intrinsic factors, such as metabolic deficiency and type III collagen mutation9,10). In young adults, it appears plausible to attribute aneurysm formation to decreased arterial durability unrelated to atherosclerosis or hypertension but rather to intrinsic arterial fragility, whereas in adult patients over the age of 40 years, ruptures may be influenced by factors such as atherosclerosis or hypertension9).
View in regard to the etiology of aneurysms is multifactorial. Degenerative hemodynamic, metabolic, and environmental factors are superimposed on congenital factors that contribute to the development of cerebral aneurysms. Hemodynamic factors are important for aneurysm formation in males. This hypothesis is supported by the fact that aneurysm development is associated with the size and complexity of the proximal ACA segment. In contrast, the intrinsic weakness of the vessel wall, collagen and elastin interference factors, and hormonal influences may play a role in aneurysm formation in women. The data in our series were obtained from a few patients to derive statistical significance and allow us to draw conclusions. Additionally, the authors did not provide any physical or histopathological evidence of increased arterial fragility to support their hypothesis regarding the pathogenesis of aneurysm formation in young adult patients9).
Surgery in young adults showed that the ruptured aneurysm was sufficiently soft and fragile to bleed prematurely but that such premature bleeding could also be easily controlled. In normotensive young adults, arterial softness and fragility may decrease the durability of arterial walls and result in aneurysm bleeding, whereas they may result in decreased bleeding at the initial stage of aneurysmal rupture. This may account for the small volume of the SAH.
5. Clinical Outcomes
Overall outcome for SAH patients under 40 was favorable; 11 patients had a GOS greater than 3 at the time of discharge, 6 patients had bad outcomes (GOS 3, 2, and 1). The rebleeding rate in good grade was low. The results of our study are consistent with those of previous reports2,7,13,15,19). In our series, the overall favorable outcome rate was 64.7% (GOS 4 and 5) and unfavorable occurred in 35.3% (GOS 2 and 3, 3 patients died). This result is lower than that of a previous study conducted by Ogunbo et al.13) (83.8%). However, when we included three patients with severe comorbidity (1 patient was in cardiac arrest, 2 patients experienced severe trauma), the number was similar (78.5%). None of the patients rebounded after clipping or endovascular treatment. Many patients continued to improve after discharge, and those in the severe and moderate disability groups showed good recovery at follow-up evaluation. Therefore, improvements are expected in young patients, and full supportive care should be continued after discharge to optimize the recovery of those with disabilities.
Generally, surgical clipping and endovascular treatment yield good outcomes in young patients. However, the durability of endovascular treatment is concerning, particularly in young adults. The same group also suggested that recoiling in the few cases in which it was mandated had a low complication rate and did not negate the original benefits of endovascular treatment. Furthermore, the advantages of initial endovascular treatment by not subjecting the injured brain to craniotomy, retraction, and other secondary injuries are likely to result in a benefit that, as suggested above, may override the risks associated with further treatment, including craniotomy for clip ligation, in a small subset of patients2).
6. Limitations of Study
This study had several limitations. First, this was a retrospective review of a small, single-institution study, which could potentially introduce bias. Second, we performed relatively short-term clinical follow-up without angiography in the endovascular group. This is an essential criterion in determining the long-term efficacy of endovascular treatment.
CONCLUSION
Our results suggest that young adults with ruptured intracranial aneurysms have better clinical outcomes. This may be due to differences in the mechanisms of aneurysmal SAH in young adults. However, further well-controlled investigations using larger prospective studies are warranted to clarify the clinical characteristics, including the mechanisms of formation and rupture, in young adults.
Notes
No potential conflict of interest relevant to this article was reported.