An Intravertebral Pseudoaneurysm Formed after Infective Spondylitis
Article information
Abstract
The surgical treatment of spondylitis involves potential risks, especially when dealing with infected tissues that may be fragile and susceptible to injury from surgical trauma and inflammation. In cases where spondylitis is not controlled even after the initial surgery, unexpected situations can arise if an unusual change in infected tissues around the spine is misinterpreted. The present case involves a 62-year-old who underwent laminectomy, debridement, and stabilization from T12 to L2 due to medically intractable spondylitis caused by methicillin-resistant Staphylococcus aureus. No major bleeding or vascular injury occurred during surgery. However, despite some improvement in pain and weakness, inflammation markers remained elevated and back pain recurred. A computed tomography (CT) scan taken 15 days after surgery showed a round-enhancing lesion inside the L1 vertebra. Although the primary imaging diagnosis suggested a loculated abscess, a round-enhancing lesion raised suspicion of an unusual pseudoaneurysm. A CT angiography confirmed a pseudoaneurysm from the L1 segmental artery, successfully treated with endovascular embolization. After embolization, the patient’s back pain improved, and inflammation markers further decreased with oral antibiotics. This case highlights the possibility of a pseudoaneurysm occurring in cases of spondylitis, emphasizing the importance of considering this entity in the differential diagnosis to ensure proper treatment.
INTRODUCTION
The primary treatment for spondylitis involves medical interventions, and surgery becomes necessary if medical treatment proves ineffective. The decision to proceed with surgery is based on clinical symptoms, laboratory findings, and imaging studies. Surgery is recommended when these results indicate that the infection is not under control4,6,8,11). Surgical procedures include laminectomy, drainage of abscess, debridement and culture of infected tissue1,4). Spinal instrumentation is performed for several objectives, such as controlling pain, restoring spinal vertebral height, correcting deformity and facilitating early ambulation. These surgical procedures are commonly employed in typical spinal surgeries. However, it is essential to be cautious, as surgical trauma and the inflammatory process can potentially cause damage to infected fragile tissues, including blood vessels19). A secondary surgery is not uncommon when spondylitis is not effectively controlled even after the first surgery. However, unexpected situations can arise if healthcare providers fail to consider unusual changes in the infected tissues surrounding the affected area. It is crucial to carefully assess the patient’s condition and monitor the response to treatment to avoid potential complications and ensure appropriate management2).
The main cause of intravertebral pseudoaneurysm is trauma, but local infection, such as spondylitis or iatrogenic trauma can also lead to the development of intravertebral pseudoaneurysm12,15,18,20). The interpretation of imaging studies for spinal infection is not simple and a paradoxical change occurred despite improved clinical and laboratory findings3,5). Therefore, a prudent interpretation is required for spinal infection, especially when a surgical treatment is considered. We experience a patient with spondylitis and a newly developed intravertebral enhancing round lesion.
CASE REPORT
A 62-years-old man had back pain (numerical rating pain scale [NRS] 5/10) and weakness (manual motor grade IV+/V on both legs) on both legs for 2 weeks due to lumbar spondylitis and bilateral psoas abscess by Methicillin-Resistant Staphylococcus aureus infection. He had underlying diabetes and end-stage renal disease requiring regular hemodialysis for more than 10 years. Medical treatment included vancomycin (10 mg/kg) and percutaneous drainage of the abscess. Medical treatment until hospital day 8, but laboratory findings showed that the infection was not medically controlled. Percutaneous drainage of the abscess was not effective. Although the assessment of the effectiveness of antibiotic treatment is limited due to its short duration, considering the patient’s symptoms, a surgical treatment plan was devised in conjunction with antibiotic therapy (Fig. 1).
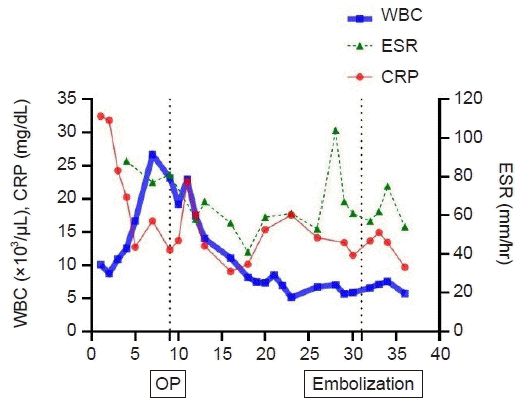
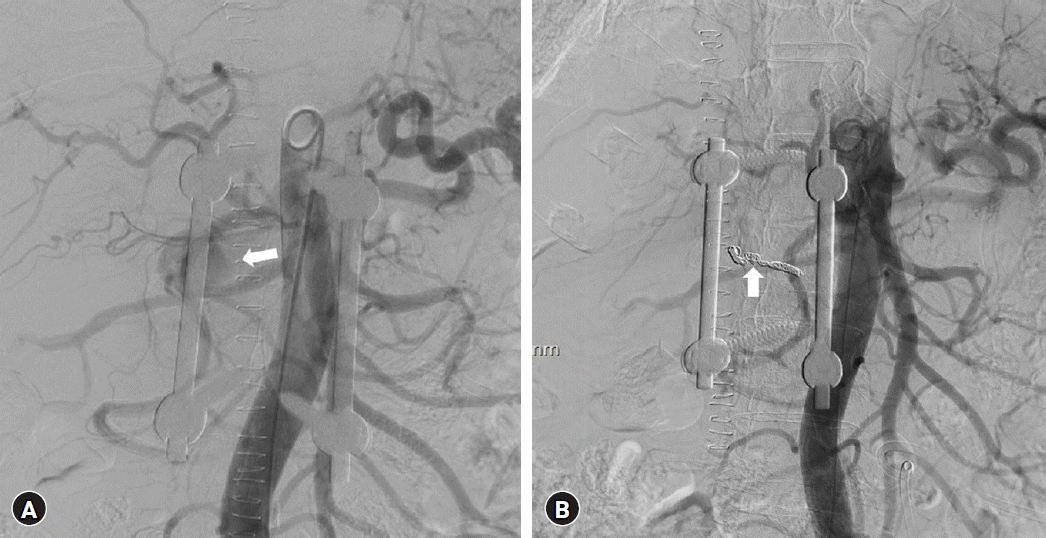
Graph showing changes in inflammatory markers during the patient’s hospital stay. Day 9 was the time of initial surgery. The time of pseudoaneurysm detection (arrow) and embolization (arrowhead) are marked in the graph. WBC: white blood cell; CRP: C-reactive protein; OP: operation; ESR: erythrocyte sedimentation rate.
He was consulted for surgical treatment. Upon physical examinations, the patient had severe tenderness on back (NRS 7/10) and weakness on both legs (manual motor grade IV-/V on both legs). He was underwent surgical treatment at the hospital on day 9. Preoperative imaging studies including magnetic resonance imaging and computed tomography scan (CT) showed spondylitis at L1, epidural abscess and abscesses in bilateral psoas (Fig. 2). Laminectomy, removal of infected epidural tissue, debridement of infected tissue inside of L1 vertebra and instrumentation from T12–L2 were performed. After surgery, vancomycin was continued, and pain and laboratory findings showed improved spondylitis with time. However, the inflammatory makers in blood were not normalized and the patient complained of relapse of back pain (NRS 10/10)
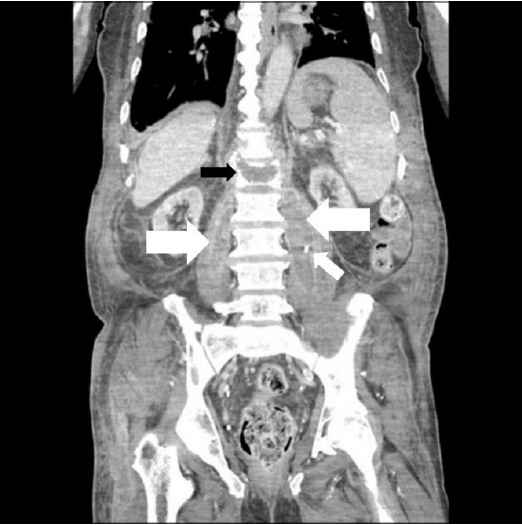
Preoperative computed tomography (CT) scan. A coronal enhanced CT scan shows spondylitis with an abscess formed along both psoas muscles (large arrows). A percutaneous drain is located in the left psoas muscle abscess (small arrow). There is no enhancing lesion inside the L1 vertebra (black arrow).
A follow-up CT scan conducted 15 days after the surgery revealed reduced abscess size in the psoas and epidural space. However, a new round-enhancing lesion was observed inside of L1 vertebra (Fig. 3A, B). The initial imaging diagnosis indicated a loculated abscess and surgery was considered a treatment option. However, a distinct, well-defined, round-shaped enhancing lesion also suggested a vascular lesion. Upon further discussion with the physician and radiologist, a pseudoaneurysm was included in the list of differential diagnosis. CT angiogram scan revealed it was a pseudoaneurysm. The pseudoaneurysm was treatment with embolization. A CT angiography revealed a pseudoaneurysm arisen from L1 segmental artery and the aneurysm was embolized with a coil on hospital day 31 (Fig. 4A, B). The back pain was improved to a tolerable level (NRS 5/10) after embolization and infection markers were decreased with continued intravenous antibiotics with adjunctive rifampin. The patient was discharged with oral suppressive antibiotics after 10 weeks of intravenous antibiotic treatment with improved back pain and leg weakness on hospital day 36 days.
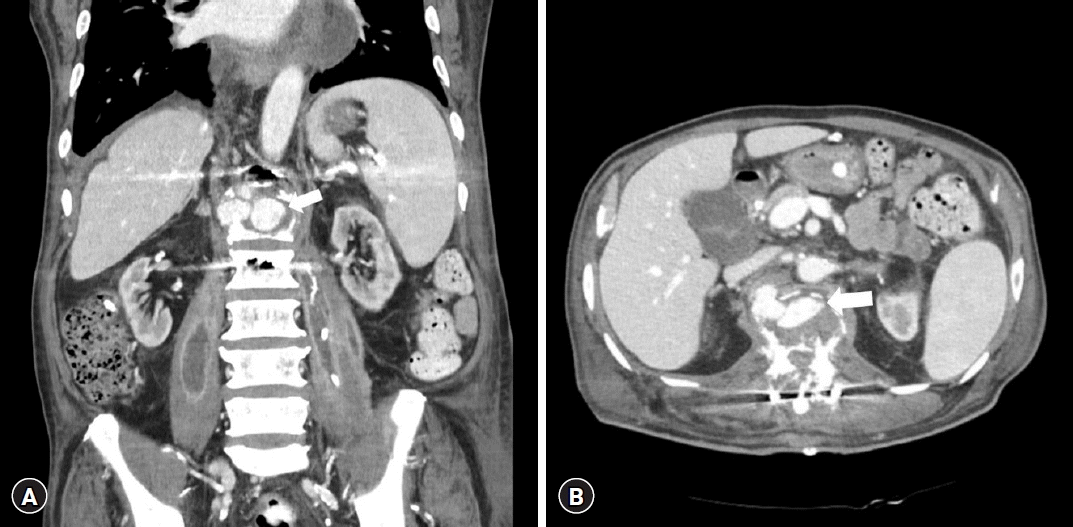
Postoperative computed tomography (CT) scan. Coronal (A) and axial (B) enhanced CT scans taken 15 days after initial surgery show a round enhancing lesion inside the L1 vertebra (arrow).
DISCUSSION
We reported a non-traumatic intravertebral pseudoaneurysm that developed in a patient with spondylitis. The exact mechanism of pseudoaneurysm formation is not clear, but it is speculated to occur due to direct surgical trauma to the segment artery or by weakening of arterial wall due to infection9,18,20). The causes of lumbar artery pseudoaneurysm were mostly direct injury to the artery such as blunt trauma, gunshot, stab injury, bleeding disorders, vertebral fracture and iatrogenic trauma such as complication of vertebral biopsy, lumbar disc surgery, and laparoscopic surgery16,17,19). A pseudoaneurysm can develop even without a direct vascular injury during surgery, owing to potential harm to the blood vessels surrounding the surgical area10,14). However, indirect injury after inflammatory process was not uncommon after infection7). In this case, the round lesion in L1 vertebra did not present before surgery and appeared after the first surgery. We did not think that a direct injury of arterial wall caused the pseudoaneurysm because arterial bleeding did not occur during the debridement of infected tissue inside L1 vertebra at the initial surgery and cortical bone of L1 vertebra was not violated. Although the exact cause of the current case was not clear, weakening of arterial wall by infection and inflammation and formation of dead space by restoration of the height of L1 vertebra and debridement of infected tissue inside of L1 vertebra, may have caused pseudoaneurysm7). If a surgical debridement was tried for the round-enhancing “abscess like” lesion, uncontrolled bleeding may have occurred during surgery. Although formation of pseudoaneurysm with spondylitis was rare, a high suspicion of pseudoaneurysm was important for proper treatment7). The treatments available for pseudoaneurysm were endovascular embolization and surgical excision. Between these two options, endovascular embolization was recommended as a primary choice due to surgical difficulties and fatal complications, such as uncontrollable intraoperative arterial bleeding13,19). In this case, we treated the pseudoaneurysm with endovascular embolization without any complications and we treated spondylitis with antibiotics.
CONCLUSION
Although the interpretation of imaging studies for spinal infection is challenging, consideration of potential life-threatening pathology should be included in the differential diagnosis. A pseudoaneurysm can develop after spondylitis and it should be considered in the differential diagnosis when a clearly margined round-enhancing lesion is observed in the vertebral body. Endovascular intervention can effectively treat the pseudoaneurysm without risk of surgical complications.
Notes
FUNDING
This study was supported by grant no. 30-2023-0120 from Seoul National University Hospital research fund. This study was supported by Doosan Yonkang foundation (800-20210527). There was no additional external funding received for this study.
No potential conflict of interest relevant to this article was reported.