INTRODUCTION
Gastrointestinal stromal tumors (GISTs) are rare mesenchymal tumors, the most common form of the gastrointestinal sarcomas accounting for 2% of all malignant gastrointestinal neoplasms7). The diagnosis of GISTs mostly relies on histopathological features and the immunohistochemical (IHC) phenotype. The most important IHC feature is the positivity of the tumor cells for CD117 and CD34. It has been reported in the literature that 90% to 95%, 60% to 70%, and 30% to 40% of GISTs express CD117, CD34, and smooth muscle actin (SMA), respectively. Only 5% are positive for S-100 protein11). Based on size, mitotic index and anatomic location, GISTs are divided into three groups with low, intermediate, and high-risk. GIST could be differentiated from other mesenchymal tumors such as schwannoma or leiomyoma, according to its distinct IHC characteristics2).
Most of the GISTs have the potential to become malignant, but, a subset of these lesions which are particularly small and asymptomatic are benign in nature14). The incidence of GIST is in the range of 20 to 40 cases per million. Over 90% of GISTs occur in adults over 40 years old, in a median age of 63 and rarely in children in the second decade (<1%)9). Most GISTs are benign; malignant tumors account for 20% to 30% of cases. Its most common anatomic sites of origin are the stomach (60%-70%), small intestine (20%-30%), colon and rectum (5%), abdominal cavity, peritoneum and omentum (5%), esophagus (<5%) and the retroperitoneal space (<3%). Patients have different symptoms, such as abdominal pain and swelling, weakness, and anemia4).
Tumor resection is the treatment of choice for localized disease. The risk of recurrence is identified by evaluating the mitotic index, dimension and site of the tumor2,7). Selective tyrosine kinase inhibitors (imatinib, sunitinib) are the standard therapy for metastatic or unresectable GISTs9). GISTs usually metastasize to the liver and peritoneum. Rare sites of metastasis are lymphnodes, lung and subcutaneous tissue, and intracranial localizations have only been described in a case report3). Bone metastases are also uncommon, and GISTs arise very rarely in the spine7).
We describe our treatment experiences of 2 cases of spinal metastases in patients with advanced GISTs.
CASE REPORT
1. Case 1
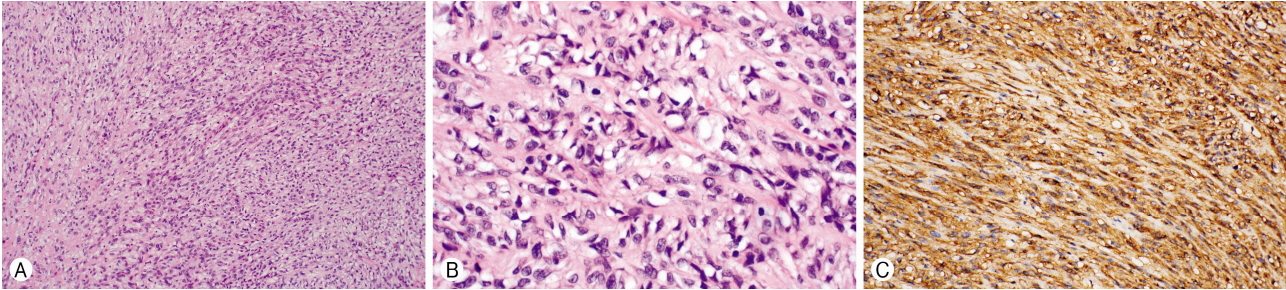
A 71-year-old female patient was examined due to abdominal discomfort developed. The examination and abdominal computed tomography (CT) scans showed a 10 cm heterogeneous mass with central necrosis and gastric ulcer at the greater curvature of the stomach. Wedge resection of the stomach and splenectomy were performed in March 2003. Results of histopathological examination showed hemorrhage and necrosis, frequent mitosis, and no metastasis in lymph nodes. According to the immunochemical analysis, C-kit and S-100 were positive, and both SMA and calponin were negative. The Ki-67 index was 20%. Tumor diameter was 17.5×12 cm. In February 2004, the patient was examined due to abdominal discomfort redeveloped. Abdominal CT scans showed multiple low attenuating nodules in the liver. Since then, imatinib mesylate 400 mg/day was given to the patient as an adjuvant treatment. The patient had complained of right buttock pain, right leg radiating pain, since February 2016. Magnetic resonance imaging (MRI) scans showed osteolytic bone destruction in the right sacrum. Increased size of soft tissue mass in right piriformis muscle and gluteus muscle across sciatic notch was observed (Fig. 1A). Furthermore, a positron emission tomography (PET)-CT scan was performed on the patient. The results showed increased activities in the right piriformis muscle, right gluteus muscles, and right sacrum (standardized uptake value[SUVmax], 8.7) (Fig. 1B). Sacral laminectomy and tumor removal were done in May 2016 (Fig. 1C). Well marginated mass lesions involving piriformis muscle, gluteus muscle and sacral body were observed. Pain complaint significantly decreased after surgery. Results of histological examination showed spinal metastasis from GIST (Fig. 2). After the surgery, the patient underwent radiosurgery to residual tumor in the sacrum. 20 gray (Gy) radiation dose in single fraction and 36 Gy radiation dose divided into 4 fractions were given to the residual tumor. The patient switched chemotherapy imatinib to sunitinib and is showing no sign of recurrence.
2. Case 2
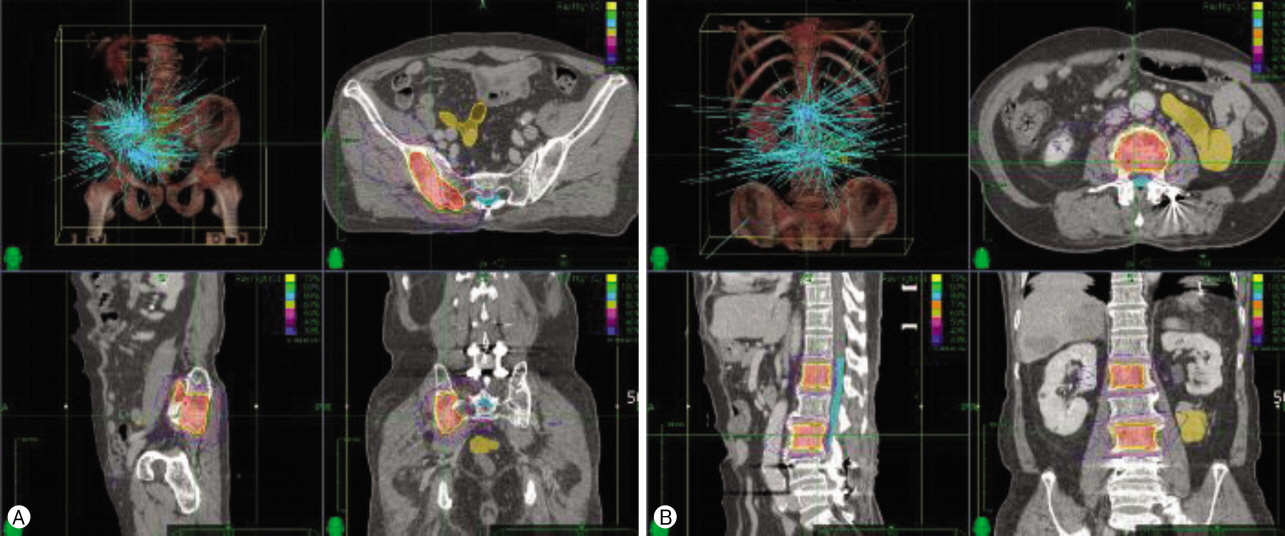
A 69-year-old male patient was examined due to abdominal discomfort. The examination and abdominal CT scans showed the presence of a about 11 cm sized a low attenuating mass in the peri-gastric area. Wedge resection of the fundus and distal pancreatectomy and omentectomy were performed in April 2009. According to the immunochemical analysis, C-kit, and CD34 were diffuse positive, both S-100 and SMA were negative. The Ki-67 index was 20%. Tumor diameter was 8.5×8 cm, and mucosal invasion was positive and resection margin was clear. Omentum was reported to have metastatic tumor involvement and lymph nodes metastasis. The pathological examination showed high-risk GIST of the stomach and omental metastasis, and lymph nodes metastasis. After the surgery, imatinib mesylate 400 mg/day was given to the patient as an adjuvant treatment. In March 2014, the patient was examined due to abdominal discomfort redeveloped. Abdominal CT scans showed mass recurrence in the retroperitoneal space. Metastasectomy was done in May 2014. The patient had complained of right buttock pain and right thigh pain from May 2017. MRI showed osteolytic bone destruction in right sacrum, pelvis and L1, L3 vertebral bodies. We performed a percutaneous needle biopsy at L3 vertebral body by kyphoplastic needle and results of pathological analysis showed spinal metastasis arising from GISTs. Since the patient had multiple metastatic lesions, it was considered impossible to remove all the lesions. Thus, we decided to perform palliative stereotactic radiosurgery (SRS). Total 36 Gy of radiation dose was given, divided 4 fractions on the spinal metastasis (Fig. 3). Pain complaints significantly decreased after the radiotherapy. After the radiosurgery, the lesions and bone scans showed decreased activities in L1 and L3 spine. In addition, the lesions in the sacrum showed no significant change. However, newly developed and increased uptake in PET scan was observed in the bilateral femur. The patient continued to undergo chemotherapy until follow-up was lost in October, 2016.
DISCUSSION
GISTs are the most common mesenchymal tumors of the gastrointestinal tract with an incidence of 10 to 20 cases per million of which almost one third are deemed malignant. The usual age at presentation is around 60. GIST may present anywhere in the gastrointestinal tract, omentum, or mesentery. The most common sites are the stomach (60%), small intestine (15%), colon and rectum (5%), other abdominal organs including mesentery, and omentum (5%)15). Metastasis is characterized by the malignant behaviors of the GIST. GISTs most frequently make metastasis to the liver and peritoneum, whereas spine and lung metastases are uncommon sites3).
Surgical removal of the tumor is currently considered to be the first choice for treatment of GIST, regardless of the presence of distant metastases2,4). Local recurrence and distant metastases have been reported to develop in more than 30% of patients with high-risk GIST despite apparently complete resections. Most recurrences or metastases occurring after resection with a R0 margin of high-risk GISTs appear within 3 years after primary surgery. An adjuvant therapy with imatinib mesylate, a specific molecular inhibitor, is beneficial after the primary GISTs are resected. Treatment for malignant GISTs using imatinib mesylate can be given at first in the treatment of advanced, recurrent, unresectable or metastatic GISTs. Once an advanced GIST (metastatic, unresectable, or recurrent) is diagnosed, imatinib should be immediately prescribed; regardless of the presence of symptoms and even if the tumor is completely resected grossly and histologically10,13). Three years of adjuvant treatment with imatinib mesylate has been shown to improve recurrence-free survival and overall survival rates in patients with high-risk GISTs6).
Bone metastases arising from GISTs have been reported, but their true prevalence is unknown. Jati et al.8) reported that 6 (3.2%), 4 and 2 of 190 GISTs patients had bone metastases, multiple bone metastases, and a solitary metastasis, respectively. The metastases involved the pelvic bone (n=4), ribs (n=4), vertebrae (n=4), and femur (n=3). The spine metastases were hypointense on T1-weighted images (WI) and hyperintense on T2-WI on MRI finding. All lesions were well-marginated and osteolytic. Except 1 patient, all lesions were discrete. There were no sclerotic components in any lesion. The metastases caused cortical disruption, which led to fractures in 2 patients. There was an associated soft tissue component in 3 patients who underwent PET. The bone metastases showed intense fluorode-oxyglucose uptake (mean SUVmax, 8.7; range, 6.7-11) which was similar to that of liver metastases (mean SUVmax, 13.4; range, 10-20).
Di Scioscio et al.5) reported 3 GIST cases with bone metastasis and two of them showed bone and liver metastasis at the time of disease presentation. The first patient had multiple osteolytic lesions in the spine and rib. The second and third patient had the lesion in the sacrum and pelvic bone. Imatinib and zoledronic acid were given to all patients. One of them received conventional radiation therapy (cRTx). Aktan et al.1) also reported the results of cRTx in 2 cases of GIST with spine metastasis. Palliative radiotherapy was performed at a fraction of 3 Gy with a total dose of 30 Gy on the spinal metastasis, and pain complaint significantly decreased after the radiotherapy.
Some of the surgical treatments of spinal metastasis in GISTs have been introduced. Waterman et al.16) reported the experience of decompression and multi-level fixation surgery in metastatic lesion at T-L spine junction with acute spinal cord compression due to aggressive regional spread. Before the surgery was performed, the origin of mass was an unknown primary malignancy lesion, and histologic results confirmed that it was GIST with spinal metastases. Slimack et al.12) also reported good surgical results in a huge metastatic lesion with spinal cord compression from GIST in the thoracic spine.
In our cases, before the surgery was performed, the patients were unable to walk due to severe radiating pain. However, after surgery was performed, the patients felt less radiating pain and were able to make ambulation. There are no complications with surgery. A surgical approach can be a treatment option in patients with spine metastasis for decompression or tumor resection. Radiosurgery or radiation therapy can be used in patients with spine metastases for palliative reasons14). In case 2, prior to radiosurgery, the patient had a severe back pain, but after the radiosurgery, the patient had shown that the back pain decreased.
CONCLUSION
We experienced two cases of spinal metastasis from GISTs and reviewed the literature. Spinal metastases from GISTs are rare, but they may become more prevalent due to increased patient life expectancy as well as the improvement in imaging techniques. GISTs should be considered in the workup of a patient with bone metastases with unknown primary malignancy. Aggressive surgical treatment is needed in metastatic lesions that cause spinal cord compression. However, SRS may be a good therapeutic option for unresectable severe metastatic lesions or patients with severe symptoms.