AbstractGuillain-Barré syndrome (GBS) is a rare immune-mediated polyneuropathy that rapidly leads to symmetric, ascending progressive weakness. Although GBS is typically associated with various infectious diseases, such as upper respiratory infections or gastroenteritis, it has also been reported following spine surgery. In this report, the authors present a case of GBS in an elderly patient after spinal fusion surgery and emphasize the importance of evaluating new-onset weakness in such cases. A 79-year-old man with diabetes mellitus and hypertension presented with weakness of the lower extremities and neurogenic claudication with chronic radicular pain. Magnetic resonance imaging revealed anterolisthesis at the L4-L5 level and disc protrusions with central and lateral recess spinal stenosis at L3-L4-L5. Following surgery, the patient complained of weakness and paresthesia in both upper extremities, prompting further investigation. An electrophysiologic study confirmed demyelinating neuropathy and cerebrospinal fluid (CSF) analysis showed elevated viral immunoglobulin levels and albumin-cytological dissociation despite negative bacterial and antiganglioside antibody tests. The patient received intravenous immunoglobulin infusion treatment and showed significant improvement, with full motor function recovery in all extremities after 6 weeks. The authors emphasize the importance of considering GBS in patients experiencing deteriorating neurological symptoms after spine surgery and suggest that electrophysiologic studies and CSF analysis are needed for an accurate diagnosis. Additionally, this report highlights the need for increased vigilance regarding the rapid onset of GBS symptoms in elderly patients following spinal surgery.
INTRODUCTIONGuillain-Barré syndrome (GBS) is a rare immune-mediated polyneuropathy characterized by rapidly progressive, symmetric, ascending weakness16). It can lead to severe conditions requiring mechanical ventilation in about 30% of cases1). The initial symptoms of GBS are diverse, including limb weakness, paresthesia, numbness, cranial nerve deficits, and pain. Although GBS is commonly associated with microbial infections like upper respiratory infections or gastroenteritis, there have been reports of it occurring after spine surgery5,8,20). The incidence of GBS after spinal surgery has been reported to be one per 2,000 cases20).
GBS diagnosis involves electrophysiology studies and cerebrospinal fluid (CSF) analysis. A decreased nerve conduction velocity (NCV) is a clinical hallmark of peripheral nerve demyelination, and albumin-cytological dissociation can assist in making the diagnosis. While there have been few reported cases of GBS after spinal surgery in elderly patients over 65 years old, this manuscript presents a case report and highlights the significance of evaluating new-onset weakness following spinal fusion surgery in this patient population.
CASE REPORTA 79-year-old man with diabetes mellitus (DM) and hypertension presented to our institution with weakness of lower extremities, neurogenic claudication with chronic radicular pain. His ability to perform daily activities was severely decreased. And he denied any history of respiratory infection and gastroenteritis. Magnetic resonance imaging (MRI) revealed anterolisthesis L4 on L5 and disc protrusions with central and lateral recess spinal stenosis on L3-4-5 level (Fig. 1). And also, bilateral foraminal stenosis due to osteoarthritis and hypertrophy of both facet joints were observed on L3-4 level (Fig. 1C). The patient was positioned prone on a Wilson frame for 5 hr and underwent L3-4-5 posterior lumbar interbody fusion for decompression of the L3, L4, and L5 nerve roots without intra-operative complications. Immediately after surgery, the motor grade of the lower extremities was above good.
The day after surgery, he reported an inability to move both legs (plantar flexion 3/3, dorsiflexion 1/1) and numbness in both feet. Moreover, he complained of weakness (3/3) and tingling sensations in both upper extremities (Table 1). We were concerned about the possibility of an epidural hematoma in the surgical field. MRI revealed a hematoma at the operative site with spinal canal stenosis (Fig. 2B). Therefore, he was taken back to the operating room, where the wound was explored, and the hematoma was removed. And additional L3 and L4 foraminotomies were performed, and the decompressed thecal sac was confirmed intra-operatively. After awakening from anesthesia, his legs were still weak, but examination revealed 3/3 plantar flexion and dorsiflexion on both sides. And deep tendon reflexes of upper and lower extremities were decreased.
The following day, he reported no improvement in upper extremity motor grade (3/3) (Table 1) and decreased fine motor activities with persistent tingling sensations. Though peripheral polyneuropathy was suspected, to rule out brain and cervical acute lesions, MR scans were performed. Brain imaging studies revealed no abnormal lesions (Fig. 2C). Cervical MRI showed mild canal stenosis without cord compression or signal changes (Fig. 2D). Subsequent electrophysiological studies, including electromyography/NCV, demonstrated electrical evidence of sensory-motor peripheral polyneuropathy in the upper (Fig. 3) and lower extremities, compatible with acute inflammatory demyelinating polyradiculoneuropathy, chronic inflammatory demyelinating polyradiculoneuropathy, or combined DM polyneuropathy.
Upon further review of the patient’s history, it was discovered that his paternal family had experienced undiagnosed neuropathy with entrapment palsies. However, genetic studies revealed no deletion of peripheral myelin protein 22 (PMP 22) associated with hereditary neuropathy with liability to pressure palsies (HNPP).
Although the CSF analysis had low reliability due to the postoperative back wound, CSF studies revealed 96 leukocyte cells/mm3, 41 erythrocyte cells/mm3, and an elevated CSF protein level of 381 mg/dL. CSF electrophoresis and anti-GM1 antibody titers were within normal limits, but an increased CSF cytomegalovirus immunoglobulin G synthesis rate of 127.2 AU/mL (normal, 0.0 - 6.0 AU/mL) was detected. Testing for Campylobacter jejuni was negative.
The patient received human immunoglobulin (I.V.-Globulin SN®; Green Cross Corp., Seoul, Korea) at 400 mg/kg for 5 days. After 6 weeks, he was discharged in a generally good condition with 5/5 distal lower extremity function. During the subsequent 12 months, he recovered all motor function without experiencing paresthesia in his hands.
DISCUSSIONIn the United States, over 300,000 spine fusions are performed annually for various purposes3). As an aging society is predicted, the number of spinal fusions is expected to increase. However, only a few cases of GBS have been reported after various spinal surgeries in the last few decades5,8,20). It is a rare but severe postoperative neurologic complication characterized by rapidly progressive inflammatory demyelinating peripheral polyneuropathy. Motor weakness, paresthesia, numbness, and even pain could be initial symptoms of GBS. The sudden and rapid escalation of GBS symptoms could make it difficult for surgeons to diagnose. Due to the unfamiliarity of surgeons with GBS, post-operative neurological deterioration is often thought of as a complication of surgery, such as nerve damage from implantation malposition, epidural hematoma, subdural hematoma, insufficient nerve decompression, etc. Some studies have shown that GBS could be triggered by various surgeries11,15). Gensicke et al.7) retrospectively demonstrated that the relative risk of GBS occurring after surgery in six weeks was 13 times higher than in the normal population. Even surgeons agonize over undiagnosed injuries of cervical cord or brain. As a result, there is a chance that patients would be misdiagnosed and improperly treated.
The initial symptoms of GBS can evolve over a period of a few hr to a week or even longer5,20). Also, the time from surgery to the onset of symptoms varies by site and type of surgery. Zhong et al.20) reported 33 GBS cases after various surgeries, including 10 cases of spinal surgery. In their study, spinal surgery showed a faster time for neurologic deficit onset than other surgeries. In our case, symptomatic motor weakness in the upper and lower extremities was reported within 16 hr of surgery, indicating a relatively rapid onset of GBS after spinal surgery.
In our case, the patient's history provided clues to suspect another rare disease, HNPP, including symptoms suggestive of entrapment neuropathy occurring among paternal family members. The pathophysiology of demyelinating sensory-motor polyneuropathy with conduction delay in the peripheral nerve of HNPP shares similarities with that of GBS. For this reason, it is difficult to differentially diagnose these two diseases with electrophysiologic study4). Additionally, HNPP could be caused by superficial peripheral nerve compression induced by the prone positioning during spine surgery performed for a relatively long time. Therefore, in this case, upper extremity motor and sensory deterioration due to HNPP were also considered. Genetic testing for the detection of a deletion or a point mutation of PMP22 genes, located at chromosome 17p11.2-12, is known as the gold standard for the diagnosis of HNPP14). However, genetic testing usually takes more time to confirm the result than CSF analysis. Therefore, in our case, it is thought that simultaneous CSF analysis could be more advantageous for the purpose of differentially diagnosing the two diseases since the results are confirmed quickly. Furthermore, in terms of cost and benefit, it is believed that CSF analysis, which is more available and cheaper, would be more advantageous. Nevertheless, it should not be overlooked that CSF analysis after spinal surgery could be difficult to interpret due to the atypical elevation of leukocyte count, erythrocyte count, and protein level in the CSF specimen caused by the inflammatory reaction of the surgical site.
Fortunately, intravenous immunoglobulin (IVIg) is known to be effective in alleviating symptoms and preventing complications in both GBS and HNPP, which are demyelinating peripheral polyneuropathies1,4,14). The randomized controlled trial of van der Meché et al.19) in 1992 first showed that the use of IVIg in GBS is as effective as plasma exchange. Since then, there have been studies proving the effectiveness of IVIg as a first treatment for GBS6,10). Therefore, for patients suspected of peripheral neuropathy progressing after spinal surgery, symptomatic treatment, including IVIg, is required, considering GBS after electrophysiology and CSF studies. Simultaneously, genetic testing is recommended for patients requiring a differential diagnosis, including HNPP, to avoid misdiagnosis and delay in diagnosis.
To the best of our knowledge, our case is the most elderly patient among the GBS cases reported so far after spinal surgery. The incidence of GBS is known to increase with age, and the disease is more common in males9). GBS is represented post-infectious auto-immune disorder caused by Campylobacter jejuni enteritis, responsible for up to half of case12). Other infectious agents include cytomrgalovirus, Epstein-Barr virus, Mycolasma pneumoniae and etc.13). The mechanisms of demyelination of peripheral nerve axons are poorly understood at the present time, but it seems that molecular mimicry between microbial antigens and axonal components plays an important role in the disease18). Several possibilities of GBS after spinal surgery could be considered in elderly patients with immunocompromised and limited activities before the surgery. First, pre-operatively, immobilized patients could be susceptible to respiratory tract infections or gastroenteritis. Second, there could be intra-operative exposure to pathogen antigens. As a result of sensitization to the antigen, triggered autoimmunization contributes to the development of GBS17). Third, damage to the nervous system from postoperative massive inflammatory reactions could provoke the release of immunogenic myelin proteins, leading to the production of antibodies2). Therefore, more special attention is needed for GBS after spinal surgery in elderly patients.
CONCLUSIONGBS is a rare but severe postoperative neurologic complication characterized by rapidly progressive inflammatory demyelinating peripheral polyneuropathy. The occurrence of GBS after spinal surgery in elderly patients warrants special attention due to the increasing incidence with age and the potential immunocompromised state of these patients. Early recognition and prompt management of GBS after spinal surgery, including IVIg treatment and genetic testing, can lead to favorable outcomes and prevent misdiagnosis or delays in treatment. It is crucial for clinicians to be vigilant and consider GBS in the postoperative evaluation of elderly patients presenting with weakness and neurologic deficits after spinal fusion surgery.
Fig. 1.Preoperative radiologic evaluation. A preoperative lateral radiograph (A) and T2-weighted sagittal magnetic resonance image (MRI) (B) of the lumbar spine show anterolisthesis of L4 on L5 and disc bulging with central spinal stenosis at the L3-4-5 levels. T2-weighted axial MRI of the L3-4 (C) and L4-5 (D) level show diffuse bulging discs with stenosis of the central and lateral recesses and bilateral foraminal stenosis with facet joint hypertrophy. 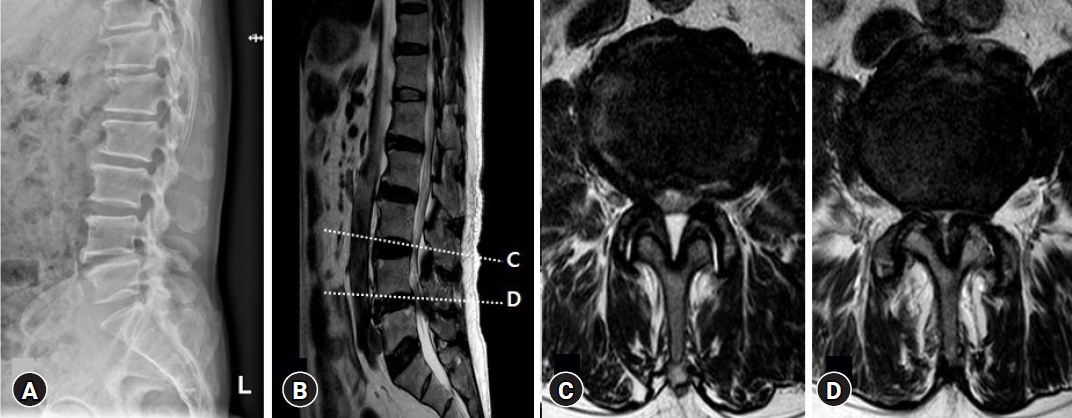
Fig. 2.Postoperative radiologic evaluation. A postoperative lateral radiograph (A) is shown. A T1-weighted magnetic resonance image (MRI) (B) shows an iso-signal hematoma (white dotted line) at operative bed with spinal canal stenosis. A T2-weighted fluid-attenuated inversion recovery MRI (C) of the brain shows no significant other abnormality except age-related white matter changes. A T2-weighted MRI (D) of the cervical spine shows mild canal stenosis without cord compression or signal change. 
Fig. 3.Electrophysiologic study. Nerve conduction studies of the right (A) and left (B) median nerves are shown. Delayed terminal latency and F-wave latency were observed. The compound muscle action potential amplitude of the elbow and axillary segment was decreased. Decreased motor nerve conduction velocity of entire segments was observed. 
Table 1.Summary of the patient’s motor grades
REFERENCES1. Atkinson SB, Carr RL, Maybee P, Haynes D: The challenges of managing and treating Guillain-Barré syndrome during the acute phase. Dimens Crit Care Nurs 25:256-263, 2006
2. Battaglia F, Sevy A, Moyse E, Roche PH: Guillain-Barré syndrome following severe head trauma and spine surgery. Rev Neurol (Paris) 169:166-168, 2013
3. Becker C: Spine-tingling prospects. Artificial disc implants are among the new technologies expected to revolutionize the outcomes of back surgery. Mod Healthc 33:30-32, 2003
4. Berciano J, Martínez-Agüeros JA, Gallardo E, Martínez-Martínez M, Infante J, García A, et al.: Hereditary neuropathy with liability to pressure palsy: fulminant radicular dysfunction during anterolateral lumbar interbody fusion. J Neurol 260:2411-2413, 2013
5. Boghani Z, Livingston AD, Simpson EP, Holman PJ, Grossman RG: Acute onset of Guillain-Barré syndrome after elective spinal surgery. World Neurosurg 84:376-379, 2015
6. Chevret S, Hughes RA, Annane D: Plasma exchange for Guillain-Barré syndrome. Cochrane Database Syst Rev 2:CD001798, 2017. Chevret S, Hughes RA, Annane D: Plasma exchange for Guillain-Barré syndrome. Cochrane Database Syst Rev 2:CD001798, 2017
7. Gensicke H, Datta AN, Dill P, Schindler C, Fischer D: Increased incidence of Guillain-Barré syndrome after surgery. Eur J Neurol 19:1239-1244, 2012
8. Huang SL, Qi HG, Liu JJ, Huang YJ, Xiang L: A rare complication of spine surgery: Guillain-Barré syndrome. World Neurosurg 84:697-701, 2015
10. Hughes RA, Swan AV, van Doorn PA: Intravenous immunoglobulin for Guillain-Barré syndrome. Cochrane Database Syst Rev 2014:CD002063, 2014
11. Ishaque N, Khealani BA, Shariff AH, Wasay M: Guillain-Barré syndrome (demyelinating) six weeks after bariatric surgery: A case report and literature review. Obes Res Clin Pract 9:416-419, 2015
12. Islam Z, Jacobs BC, van Belkum A, Mohammad QD, Islam MB, Herbrink P, et al.: Axonal variant of Guillain-Barre syndrome associated with Campylobacter infection in Bangladesh. Neurology 74:581-587, 2010
13. Jacobs BC, Rothbarth PH, van der Meché FG, Herbrink P, Schmitz PI, de Klerk MA, et al.: The spectrum of antecedent infections in Guillain-Barré syndrome: a case-control study. Neurology 51:1110-1115, 1998
14. Moerman CJ, Van Havenbergh T, Van Houwe P, Casaer S: Management of anesthesia for surgery in prone position for a patient with hereditary neuropathy with liability to pressure palsies. A case report and narrative literature review. Acta Anaesthesiol Belg 72:145-149, 2021
15. Rashid A, Kurra S, Lavelle W: Guillain-Barré syndrome after revision lumbar surgery: A case report. Cureus 9:e1393. 2017
16. Sejvar JJ, Baughman AL, Wise M, Morgan OW: Population incidence of Guillain-Barré syndrome: a systematic review and meta-analysis. Neuroepidemiology 36:123-133, 2011
17. Steiner I, Argov Z, Cahan C, Abramsky O: Guillain-Barré syndrome after epidural anesthesia: direct nerve root damage may trigger disease. Neurology 35:1473-1475, 1985
18. Susuki K, Yuki N, Schafer DP, Hirata K, Zhang G, Funakoshi K, et al.: Dysfunction of nodes of Ranvier: a mechanism for anti-ganglioside antibody-mediated neuropathies. Exp Neurol 233:534-542, 2012
19. van der Meché FG, Schmitz PI: A randomized trial comparing intravenous immune globulin and plasma exchange in Guillain-Barré syndrome. Dutch Guillain-Barré Study Group. N Engl J Med 326:1123-1129, 1992
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||